

Scientists have found that alcohol can trigger migraines through several mechanisms, including dehydration, vasodilation, effects of additives, and disruption of sleep patterns.
Ready to say goodbye to alcohol-induced migraines for good? The Reframe app can help! While we’re not a cure for alcohol use disorder (AUD), we can help you cut back on drinking gradually by using science-backed methods to empower you throughout your journey. Our program has helped millions of people just like you to drink less and live more!
The Reframe app gives you the tools and knowledge to cut back or quit drinking less in an intuitive, effective way. You’ll receive daily science-backed readings and will have access to our in-app Toolkit, filled with the resources and activities you need to navigate anything life throws at you.
You’ll meet millions of fellow Reframers in our 24/7 Forum chat and daily Zoom check-in meetings. Receive encouragement from people worldwide who know exactly what you’re going through! You’ll also have the opportunity to connect with our licensed Reframe coaches for more personalized guidance.
Plus, we’re always introducing new features to optimize your in-app experience. We recently launched our in-app chatbot, Melody, powered by the world’s most powerful AI technology. Melody is here to help as you adjust to a life with less (or no) alcohol.
And that’s not all! Every month, we launch fun challenges, like Dry/Damp January, Mental Health May, and Outdoorsy June. You won’t want to miss out on the chance to participate alongside fellow Reframers (or solo if that’s more your thing!).
The Reframe app is free for 7 days, so you don’t have anything to lose by trying it. Are you ready to feel empowered and discover life beyond alcohol? Then download our app through the App Store or Google Play today!
Alcohol can be a real conundrum for those of us who get migraines. Perhaps you've experienced that splitting headache after a night of indulgence. Let's delve into the world of migraine research and explore how alcohol might be a contributing factor.
When we think about migraines, we often picture intense, throbbing headaches. But migraines are often accompanied by a whole carnival of symptoms — including nausea, sensitivity to light and sound, and sometimes visual disturbances known as “auras.”
What happens when alcohol enters the equation? We're all familiar with the infamous “hangover headache,” but can alcohol cause migraines? And what’s the connection between cocktails and headaches?
In a word: yes. Research studies have shown that alcohol can, indeed, act as a migraine trigger for some people. But why does this happen? The answer lies in the way alcohol interacts with our bodies.
A growing body of scientific research suggests a possible connection between alcohol consumption and migraines. A 2018 study found that alcohol was reported to be a trigger in 35.6% of migraine patients. However, the relationship between alcohol and migraines is complex, involving several scientific theories.
First off, alcohol is a diuretic: it encourages our kidneys to produce more urine, leading to dehydration. Since dehydration is a well-known trigger for migraines, it's no surprise that our beloved drinks can push us towards a throbbing headache.
Moreover, alcohol can cause blood vessels in our brain to expand, a process called vasodilation. This change in the body's internal roadways can trigger migraines in some people.
But the story doesn't end there. Alcohol — especially dark drinks such as red wine and whiskey — contain chemicals known as congeners, which can set off migraines for some of us.
Finally, alcohol affects our sleep patterns. Even though a couple of drinks might make us feel sleepy, they actually disrupt our sleep cycle, causing poor sleep quality over the course of the night. Our brains don't appreciate this, and they often retaliate with a migraine.

It's important to distinguish between a “cause” and a “trigger.” The cause of migraines is multifaceted, often involving genetic factors and imbalances in brain chemicals. Alcohol is not a “cause” of migraines per se, but it can be a “trigger” for migraine attacks in those of us prone to them for other reasons.
Red wine is widely believed to be a major offender. However, research has demonstrated that all types of alcoholic beverages can trigger migraines. A study in the European Journal of Neurology found that while red wine was the most frequently reported trigger, other alcoholic drinks were not far behind.
It's essential to note that everyone's experience with alcohol and migraines is unique. Some of us may have a migraine episode after just a single glass of champagne, while others may not experience any adverse effects even after consuming multiple drinks. This variability is attributed to our individual genetic makeup, lifestyle factors, and the type of alcohol consumed.
For those of us who are frequent drinkers and are considering quitting, it's important to understand that alcohol withdrawal may trigger migraines, too. This is because our brain has adapted to the regular presence of alcohol and reacts to its absence. This is only a factor until our brain becomes accustomed to life without alcohol, so don’t let this deter you from quitting, if that’s your goal.
So, what can we do about the migraine-alcohol connection? Here are some specific action steps for those of us considering cutting back on or quitting alcohol.
Everyone’s journey towards a migraine-free future is unique. While it may seem like a tall order, armed with knowledge and determination, we can take a step towards it by managing our alcohol intake. Remember, alcohol is not the only potential trigger for migraines. A holistic lifestyle change, which includes balanced nutrition, regular exercise, and stress management, along with reducing alcohol consumption, can have a profound impact on our overall well-being.
Alcohol can be a real conundrum for those of us who get migraines. Perhaps you've experienced that splitting headache after a night of indulgence. Let's delve into the world of migraine research and explore how alcohol might be a contributing factor.
When we think about migraines, we often picture intense, throbbing headaches. But migraines are often accompanied by a whole carnival of symptoms — including nausea, sensitivity to light and sound, and sometimes visual disturbances known as “auras.”
What happens when alcohol enters the equation? We're all familiar with the infamous “hangover headache,” but can alcohol cause migraines? And what’s the connection between cocktails and headaches?
In a word: yes. Research studies have shown that alcohol can, indeed, act as a migraine trigger for some people. But why does this happen? The answer lies in the way alcohol interacts with our bodies.
A growing body of scientific research suggests a possible connection between alcohol consumption and migraines. A 2018 study found that alcohol was reported to be a trigger in 35.6% of migraine patients. However, the relationship between alcohol and migraines is complex, involving several scientific theories.
First off, alcohol is a diuretic: it encourages our kidneys to produce more urine, leading to dehydration. Since dehydration is a well-known trigger for migraines, it's no surprise that our beloved drinks can push us towards a throbbing headache.
Moreover, alcohol can cause blood vessels in our brain to expand, a process called vasodilation. This change in the body's internal roadways can trigger migraines in some people.
But the story doesn't end there. Alcohol — especially dark drinks such as red wine and whiskey — contain chemicals known as congeners, which can set off migraines for some of us.
Finally, alcohol affects our sleep patterns. Even though a couple of drinks might make us feel sleepy, they actually disrupt our sleep cycle, causing poor sleep quality over the course of the night. Our brains don't appreciate this, and they often retaliate with a migraine.

It's important to distinguish between a “cause” and a “trigger.” The cause of migraines is multifaceted, often involving genetic factors and imbalances in brain chemicals. Alcohol is not a “cause” of migraines per se, but it can be a “trigger” for migraine attacks in those of us prone to them for other reasons.
Red wine is widely believed to be a major offender. However, research has demonstrated that all types of alcoholic beverages can trigger migraines. A study in the European Journal of Neurology found that while red wine was the most frequently reported trigger, other alcoholic drinks were not far behind.
It's essential to note that everyone's experience with alcohol and migraines is unique. Some of us may have a migraine episode after just a single glass of champagne, while others may not experience any adverse effects even after consuming multiple drinks. This variability is attributed to our individual genetic makeup, lifestyle factors, and the type of alcohol consumed.
For those of us who are frequent drinkers and are considering quitting, it's important to understand that alcohol withdrawal may trigger migraines, too. This is because our brain has adapted to the regular presence of alcohol and reacts to its absence. This is only a factor until our brain becomes accustomed to life without alcohol, so don’t let this deter you from quitting, if that’s your goal.
So, what can we do about the migraine-alcohol connection? Here are some specific action steps for those of us considering cutting back on or quitting alcohol.
Everyone’s journey towards a migraine-free future is unique. While it may seem like a tall order, armed with knowledge and determination, we can take a step towards it by managing our alcohol intake. Remember, alcohol is not the only potential trigger for migraines. A holistic lifestyle change, which includes balanced nutrition, regular exercise, and stress management, along with reducing alcohol consumption, can have a profound impact on our overall well-being.

Learn how alcohol and cancer are connected, the science behind the risk, and practical steps you can take to protect your long-term health.
Although it isn’t a treatment for alcohol use disorder (AUD), the Reframe app can help you cut back on drinking gradually, with the science-backed knowledge to empower you 100% of the way. Our proven program has helped millions of people around the world drink less and live more. And we want to help you get there, too!
The Reframe app equips you with the knowledge and skills you need to not only survive drinking less, but to thrive while you navigate the journey. Our daily research-backed readings teach you the neuroscience of alcohol, and our in-app Toolkit provides the resources and activities you need to navigate each challenge.
You’ll meet millions of fellow Reframers in our 24/7 Forum chat and daily Zoom check-in meetings. Receive encouragement from people worldwide who know exactly what you’re going through! You’ll also have the opportunity to connect with our licensed Reframe coaches for more personalized guidance.
Plus, we’re always introducing new features to optimize your in-app experience. We recently launched our in-app chatbot, Melody, powered by the world’s most powerful AI technology. Melody is here to help as you adjust to a life with less (or no) alcohol.
And that’s not all! Every month, we launch fun challenges, like Dry/Damp January, Mental Health May, and Outdoorsy June. You won’t want to miss out on the chance to participate alongside fellow Reframers (or solo if that’s more your thing!).
The Reframe app is free for 7 days, so you don’t have anything to lose by trying it. Are you ready to feel empowered and discover life beyond alcohol? Then download our app through the App Store or Google Play today!
A glass of wine after a long day can feel like a simple pleasure, right? We often hear about alcohol's effect on the liver, but there's a quieter, more serious conversation we need to have about alcohol and cancer. The truth is, the risk is real, even for moderate drinkers. The process of alcohol causing cancer starts the moment you take a sip, as your body breaks it down into a harmful chemical. Let's look at the facts behind the alcohol and cancer risk so you can make informed choices for your health.
When we talk about the health effects of alcohol, we often think of liver damage or addiction. But the conversation is shifting to include a significant, and often overlooked, connection to cancer. It’s a heavy topic, I know, but understanding the science is the first step toward making informed choices for our health. The evidence isn't just correlational; major health organizations have identified alcohol as a carcinogen, meaning it has the potential to cause cancer. This happens through a few different mechanisms, like how our bodies break down alcohol into a toxic chemical called acetaldehyde, which can damage our DNA and stop our cells from repairing themselves. It’s not about fear, but about awareness and empowerment.
So, which cancers are we talking about? The list is more extensive than many people realize. According to health authorities like the CDC, drinking alcohol raises your risk for several types of cancer. This includes cancers of the mouth, throat, and voice box (larynx). It doesn't stop there; the risk extends to the esophagus, colon and rectum, and liver. For women, alcohol consumption is also a known risk factor for breast cancer. The connection is clear and well-documented, showing that alcohol can affect various parts of the body, particularly along the digestive tract where it comes into direct contact with tissues. Knowing exactly where the risks lie helps to create a fuller picture of alcohol's impact on our long-term health.
The numbers behind this connection are pretty sobering. Research shows that alcohol is a significant contributor to both cancer cases and cancer deaths globally. In the United States alone, about 20,000 adults die each year from cancers linked to alcohol. To put it another way, roughly 5.5% of all new cancer cases are associated with drinking. The risk also increases with the amount you drink. For example, drinking about 3.5 drinks per day can double or even triple your risk for cancers of the mouth and throat. These statistics aren't meant to scare you, but to highlight the real-world impact. This knowledge can be a powerful motivator for anyone looking to re-evaluate their habits and explore a more mindful approach to drinking.
Is alcohol a carcinogen? Yes, but the real risk is its metabolite, acetaldehyde. When we consume alcohol, our bodies set out to break it down, primarily in the liver. In this process, a compound called acetaldehyde is formed. Acetaldehyde is a bit of a rascal. It's a carcinogen, which means it can cause cancer by damaging DNA and stopping our cells from repairing this damage. Over time, this can lead to abnormal cell growth, potentially developing into cancer.
Let’s look into the mechanics of acetaldehyde in a bit more detail. The International Agency for Research on Cancer has classified this volatile compound in the highest risk category: it’s a Group 1 carcinogen alongside substances like tobacco smoke and asbestos.
But how exactly does acetaldehyde contribute to cancer development? There are several ways it exerts its harmful effects:
Our bodies do have defense mechanisms against acetaldehyde, such as the enzyme aldehyde dehydrogenase (ALDH), which breaks down acetaldehyde into a non-toxic substance. However, certain individuals have a variant of the ALDH enzyme that works less efficiently, leading to a flushed complexion and an accumulation of acetaldehyde after drinking. This population may have a higher risk of alcohol-related cancers.

As we’ve touched on, acetaldehyde is the primary villain in this story. This toxic chemical directly attacks our DNA, the very instruction manual for our cells. It creates what scientists call “DNA adducts,” which are essentially harmful attachments that distort our DNA’s structure. Think of it like a typo in a critical line of code. When our cells try to replicate with this damaged code, it can lead to mutations. These mutations can cause cells to grow uncontrollably, which is the hallmark of cancer. This direct damage is one of the most significant ways alcohol consumption increases cancer risk, fundamentally altering our cellular blueprints over time.
It’s easy to forget that alcoholic drinks can be packed with calories, often with little to no nutritional value. These "empty calories" can contribute to weight gain, and carrying excess body weight is a well-established risk factor for several types of cancer, including breast, colon, and pancreatic cancer. Alcohol can also lower our inhibitions and stimulate appetite, leading to poor food choices. The connection is straightforward: regular drinking can make it harder to maintain a healthy weight, and that extra weight creates an environment in the body that’s more favorable for cancer to develop. You can get a clearer picture of your own consumption by using a tool to calculate the calories in the drinks you have.
Our liver is a powerhouse organ, responsible for filtering toxins from our blood, and alcohol is one of the biggest toxins it has to process. Heavy or consistent drinking puts immense strain on the liver, leading to inflammation and cell damage. Over time, this can result in a condition called cirrhosis, where healthy liver tissue is replaced by scar tissue. This scarring severely impairs liver function and dramatically increases the risk of developing liver cancer. Essentially, by overwhelming the liver, alcohol creates the very conditions—damage and scarring—that can pave the way for malignant cells to grow.
Drinking alcohol doesn't just add harmful substances to your body; it also hinders your body's ability to absorb the good stuff. Alcohol can irritate the lining of the stomach and intestines, which interferes with the absorption of essential vitamins and nutrients from the food you eat. One of the most critical nutrients affected is folate, a B vitamin that is vital for creating and repairing DNA. When your body is low on folate, it’s less equipped to fix the DNA damage caused by factors like acetaldehyde. This nutritional deficiency weakens your body's natural cancer defenses, making cells more vulnerable to mutations.
Inflammation is your body's natural response to injury or infection—a short-term defense mechanism. However, when your body is constantly exposed to irritants like alcohol, this response can become chronic. This state of ongoing, low-grade inflammation can be incredibly damaging. It produces free radicals that can harm your DNA, and it signals cells to divide more rapidly to repair the damage. This constant cycle of damage and rapid regeneration increases the chances of errors occurring during cell division, which can ultimately lead to the formation of cancerous tumors. Chronic inflammation essentially creates a fertile ground for cancer to take root and grow.
Alcohol also impacts hormone levels, especially sex hormones such as estrogen and testosterone. These hormonal imbalances are another route by which alcohol can increase cancer risk — particularly breast cancer. Breast cancer and alcohol have a well-established relationship. Let’s discuss the connection!
In women, estrogen promotes the development and maintenance of female characteristics, but it also regulates the growth and division of breast cells. Consuming alcohol can increase levels of estrogen in the body. A higher estrogen level means more cell divisions in breast tissue, increasing the likelihood of mutations and the development of cancer cells. Some of these cell divisions can lead to mutations, and over time, these mutations can accumulate and result in cancer.
Alcohol can also impact other hormones. For instance, it can raise levels of the hormone insulin-like growth factor 1 (IGF-1), which encourages cells to divide. Higher levels of IGF-1 have been associated with an increased risk of certain cancers, including breast and prostate cancer.
Additionally, alcohol can affect the liver's ability to regulate hormone levels due to the liver's role in detoxifying alcohol and metabolizing hormones. This can lead to hormonal imbalances and further increase the risk of cancer.
The hormonal effects of alcohol contribute to the risk of several cancers. Apart from breast cancer, alcohol-related hormonal imbalances can increase the risk of ovarian and endometrial cancers in women, and possibly prostate cancer in men.
So, why does alcohol pose a greater cancer risk for women? It largely comes down to our unique physiology and how our bodies process alcohol. Women generally have less body water than men of the same weight, which means alcohol becomes more concentrated in our system. On top of that, our stomachs produce less of the enzyme that breaks down alcohol before it even reaches the bloodstream. This combination means we absorb more alcohol and it takes longer to metabolize, leading to more prolonged exposure to the carcinogen acetaldehyde. This increased exposure, combined with alcohol’s tendency to disrupt our hormonal health, creates a perfect storm that elevates the risk for cancers of the breast, ovaries, and endometrium.
In addition to triggering these internal mechanisms, alcohol can increase cancer risk indirectly by making it easier for other harmful processes to take place.
Alcohol can act as a solvent, making it easier for carcinogenic chemicals — such as tobacco smoke — to enter our cells. It can also weaken our immune system, making it harder for us to fight off diseases, including cancer.
We’ve all heard it, right? That a glass of red wine with dinner is actually good for you, especially your heart. But this popular belief often glosses over a much more serious reality: the significant cancer risks tied to drinking any kind of alcohol. The truth is, when it comes to cancer, your body doesn't distinguish between a fancy Merlot and a cheap beer. The common denominator in all alcoholic drinks is ethanol, and that's where the trouble begins. All types of alcohol, whether it's wine, beer, or liquor, carry the same cancer risk because they all contain this compound.
So, what about drinking in moderation? Unfortunately, experts are clear that there is no safe amount of alcohol when it comes to cancer. Even a small amount increases your risk. While some studies have pointed to potential heart benefits from the antioxidants in red wine, these benefits simply don't outweigh the proven cancer risks. The more alcohol you consume, the higher your risk becomes. It's a straightforward relationship that puts the "healthy glass of wine" idea into a much different perspective, encouraging us to look at the complete picture of how alcohol affects our long-term health.
So how can we use this information to live healthier lives? For one, cutting back on alcohol or abstaining altogether can significantly reduce our risk.
Here are some additional changes that can make a big difference:
Together, we can navigate the journey to a healthier, happier life. Remember, every little step counts!
When it comes to alcohol and health, it helps to have a clear benchmark. Official guidelines from health organizations like the Centers for Disease Control and Prevention (CDC) provide a framework based on scientific evidence. These recommendations aren't about judgment; they're about giving you the information you need to make choices that align with your health goals. Understanding what experts consider moderate consumption is a crucial first step in evaluating your own habits. It allows you to see where you stand and decide what, if any, changes you’d like to make. Think of it as a map — it shows you the terrain so you can choose your path forward.
One of the biggest hurdles in tracking alcohol intake is knowing what a “standard drink” actually is. It’s easy to underestimate how much you’re consuming when drink sizes vary so much. According to the MD Anderson Cancer Center, one standard drink is defined as 12 ounces of beer, 5 ounces of wine, or 1.5 ounces of 80-proof liquor. That generous glass of wine you pour at home could easily count as two standard drinks. Being aware of these measurements is key to accurately assessing your consumption and understanding your risk. It’s the foundation of mindful drinking and helps you stay honest with yourself about your habits.
So, what do the experts recommend? The CDC advises that if you choose to drink, you do so in moderation. For women, this means one standard drink or less per day, and for men, it’s two standard drinks or less per day. It’s important to remember that these are upper limits for the days you do drink, not daily targets to aim for. The healthiest option is always to drink less. These guidelines are designed to help minimize health risks, including the risk of cancer. Sticking to them is a powerful way to protect your long-term well-being while still allowing yourself to enjoy a drink on occasion if you choose to.
The link between how much you drink and your cancer risk is direct and significant. It’s not just heavy drinking that poses a threat; even moderate amounts can increase your chances of developing certain cancers. According to the Canadian Cancer Society, consuming about 3.5 drinks a day can double or even triple your risk of cancers in the mouth, throat, and esophagus. The same amount increases the risk of colon and breast cancer by 1.5 times. This dose-response relationship is clear: the more you drink, the higher your risk. This knowledge is empowering because it puts the control back in your hands. Every drink you skip is a step toward lowering that risk.
If you're feeling concerned, here’s some good news: it’s never too late to make a positive change. When you stop drinking, your risk for alcohol-related cancers begins to decrease over time. While it may take many years for the risk to be fully removed, quitting is a significant and proactive step for your health. Your body has an incredible capacity for healing, and reducing its exposure to carcinogens like acetaldehyde gives it a chance to repair. This journey of mindful drinking or quitting entirely is one of the most impactful things you can do for your future self, and every day alcohol-free is a victory for your long-term health.
For anyone currently facing a cancer diagnosis or in recovery, the conversation around alcohol becomes even more critical. It’s essential to talk to your doctor about your alcohol use. Drinking can interfere with treatment, worsen side effects, and potentially increase the risk of developing new cancers. Your healthcare team can provide personalized advice based on your specific diagnosis, treatment plan, and overall health. This conversation is a vital part of your care, ensuring that your lifestyle choices support your recovery and help protect your health moving forward. Don't hesitate to bring it up; your medical team is there to support you in every aspect of your journey.
I've always heard that a glass of red wine is good for you. Is that not true when it comes to cancer? That's a common belief, but when we're talking about cancer risk, the type of alcohol doesn't matter. Whether it's wine, beer, or liquor, they all contain ethanol, which your body converts into a cancer-causing chemical. While some studies point to antioxidants in red wine for heart health, those benefits don't cancel out the proven cancer risk that comes with any alcoholic drink.
Does even light or moderate drinking really increase my cancer risk? Yes, unfortunately, the evidence is clear that even small amounts of alcohol can increase your risk for certain cancers. There isn't a "safe" threshold when it comes to cancer prevention. The relationship is straightforward: the more you drink over time, the higher your risk becomes. This is why understanding what a standard drink is and being mindful of your intake is so important.
Why is the cancer risk from alcohol higher for women? It really comes down to our physiology. Women tend to have less body water than men, which means alcohol becomes more concentrated in our systems. We also produce less of a key enzyme in our stomachs that breaks down alcohol. This combination leads to higher blood alcohol concentrations and longer exposure to its harmful byproducts, which, along with alcohol's effect on hormones like estrogen, elevates our risk.
What is the main way alcohol actually causes cancer? The primary culprit is a toxic chemical called acetaldehyde. When you drink alcohol, your body works to break it down, and acetaldehyde is the main byproduct of that process. This chemical is a known carcinogen that can directly damage the DNA in your cells and prevent your body from repairing that damage. Over time, this can lead to mutations that cause cells to grow uncontrollably.
If I cut back or stop drinking now, can I actually lower my risk? Absolutely. It's one of the most empowering things to know. While it can take time, your body has an amazing ability to heal. When you reduce or eliminate alcohol, you lower your exposure to its cancer-causing effects, and your risk for developing alcohol-related cancers begins to decrease. Every step you take toward drinking less is a positive move for your long-term health.
A glass of wine after a long day can feel like a simple pleasure, right? We often hear about alcohol's effect on the liver, but there's a quieter, more serious conversation we need to have about alcohol and cancer. The truth is, the risk is real, even for moderate drinkers. The process of alcohol causing cancer starts the moment you take a sip, as your body breaks it down into a harmful chemical. Let's look at the facts behind the alcohol and cancer risk so you can make informed choices for your health.
When we talk about the health effects of alcohol, we often think of liver damage or addiction. But the conversation is shifting to include a significant, and often overlooked, connection to cancer. It’s a heavy topic, I know, but understanding the science is the first step toward making informed choices for our health. The evidence isn't just correlational; major health organizations have identified alcohol as a carcinogen, meaning it has the potential to cause cancer. This happens through a few different mechanisms, like how our bodies break down alcohol into a toxic chemical called acetaldehyde, which can damage our DNA and stop our cells from repairing themselves. It’s not about fear, but about awareness and empowerment.
So, which cancers are we talking about? The list is more extensive than many people realize. According to health authorities like the CDC, drinking alcohol raises your risk for several types of cancer. This includes cancers of the mouth, throat, and voice box (larynx). It doesn't stop there; the risk extends to the esophagus, colon and rectum, and liver. For women, alcohol consumption is also a known risk factor for breast cancer. The connection is clear and well-documented, showing that alcohol can affect various parts of the body, particularly along the digestive tract where it comes into direct contact with tissues. Knowing exactly where the risks lie helps to create a fuller picture of alcohol's impact on our long-term health.
The numbers behind this connection are pretty sobering. Research shows that alcohol is a significant contributor to both cancer cases and cancer deaths globally. In the United States alone, about 20,000 adults die each year from cancers linked to alcohol. To put it another way, roughly 5.5% of all new cancer cases are associated with drinking. The risk also increases with the amount you drink. For example, drinking about 3.5 drinks per day can double or even triple your risk for cancers of the mouth and throat. These statistics aren't meant to scare you, but to highlight the real-world impact. This knowledge can be a powerful motivator for anyone looking to re-evaluate their habits and explore a more mindful approach to drinking.
Is alcohol a carcinogen? Yes, but the real risk is its metabolite, acetaldehyde. When we consume alcohol, our bodies set out to break it down, primarily in the liver. In this process, a compound called acetaldehyde is formed. Acetaldehyde is a bit of a rascal. It's a carcinogen, which means it can cause cancer by damaging DNA and stopping our cells from repairing this damage. Over time, this can lead to abnormal cell growth, potentially developing into cancer.
Let’s look into the mechanics of acetaldehyde in a bit more detail. The International Agency for Research on Cancer has classified this volatile compound in the highest risk category: it’s a Group 1 carcinogen alongside substances like tobacco smoke and asbestos.
But how exactly does acetaldehyde contribute to cancer development? There are several ways it exerts its harmful effects:
Our bodies do have defense mechanisms against acetaldehyde, such as the enzyme aldehyde dehydrogenase (ALDH), which breaks down acetaldehyde into a non-toxic substance. However, certain individuals have a variant of the ALDH enzyme that works less efficiently, leading to a flushed complexion and an accumulation of acetaldehyde after drinking. This population may have a higher risk of alcohol-related cancers.

As we’ve touched on, acetaldehyde is the primary villain in this story. This toxic chemical directly attacks our DNA, the very instruction manual for our cells. It creates what scientists call “DNA adducts,” which are essentially harmful attachments that distort our DNA’s structure. Think of it like a typo in a critical line of code. When our cells try to replicate with this damaged code, it can lead to mutations. These mutations can cause cells to grow uncontrollably, which is the hallmark of cancer. This direct damage is one of the most significant ways alcohol consumption increases cancer risk, fundamentally altering our cellular blueprints over time.
It’s easy to forget that alcoholic drinks can be packed with calories, often with little to no nutritional value. These "empty calories" can contribute to weight gain, and carrying excess body weight is a well-established risk factor for several types of cancer, including breast, colon, and pancreatic cancer. Alcohol can also lower our inhibitions and stimulate appetite, leading to poor food choices. The connection is straightforward: regular drinking can make it harder to maintain a healthy weight, and that extra weight creates an environment in the body that’s more favorable for cancer to develop. You can get a clearer picture of your own consumption by using a tool to calculate the calories in the drinks you have.
Our liver is a powerhouse organ, responsible for filtering toxins from our blood, and alcohol is one of the biggest toxins it has to process. Heavy or consistent drinking puts immense strain on the liver, leading to inflammation and cell damage. Over time, this can result in a condition called cirrhosis, where healthy liver tissue is replaced by scar tissue. This scarring severely impairs liver function and dramatically increases the risk of developing liver cancer. Essentially, by overwhelming the liver, alcohol creates the very conditions—damage and scarring—that can pave the way for malignant cells to grow.
Drinking alcohol doesn't just add harmful substances to your body; it also hinders your body's ability to absorb the good stuff. Alcohol can irritate the lining of the stomach and intestines, which interferes with the absorption of essential vitamins and nutrients from the food you eat. One of the most critical nutrients affected is folate, a B vitamin that is vital for creating and repairing DNA. When your body is low on folate, it’s less equipped to fix the DNA damage caused by factors like acetaldehyde. This nutritional deficiency weakens your body's natural cancer defenses, making cells more vulnerable to mutations.
Inflammation is your body's natural response to injury or infection—a short-term defense mechanism. However, when your body is constantly exposed to irritants like alcohol, this response can become chronic. This state of ongoing, low-grade inflammation can be incredibly damaging. It produces free radicals that can harm your DNA, and it signals cells to divide more rapidly to repair the damage. This constant cycle of damage and rapid regeneration increases the chances of errors occurring during cell division, which can ultimately lead to the formation of cancerous tumors. Chronic inflammation essentially creates a fertile ground for cancer to take root and grow.
Alcohol also impacts hormone levels, especially sex hormones such as estrogen and testosterone. These hormonal imbalances are another route by which alcohol can increase cancer risk — particularly breast cancer. Breast cancer and alcohol have a well-established relationship. Let’s discuss the connection!
In women, estrogen promotes the development and maintenance of female characteristics, but it also regulates the growth and division of breast cells. Consuming alcohol can increase levels of estrogen in the body. A higher estrogen level means more cell divisions in breast tissue, increasing the likelihood of mutations and the development of cancer cells. Some of these cell divisions can lead to mutations, and over time, these mutations can accumulate and result in cancer.
Alcohol can also impact other hormones. For instance, it can raise levels of the hormone insulin-like growth factor 1 (IGF-1), which encourages cells to divide. Higher levels of IGF-1 have been associated with an increased risk of certain cancers, including breast and prostate cancer.
Additionally, alcohol can affect the liver's ability to regulate hormone levels due to the liver's role in detoxifying alcohol and metabolizing hormones. This can lead to hormonal imbalances and further increase the risk of cancer.
The hormonal effects of alcohol contribute to the risk of several cancers. Apart from breast cancer, alcohol-related hormonal imbalances can increase the risk of ovarian and endometrial cancers in women, and possibly prostate cancer in men.
So, why does alcohol pose a greater cancer risk for women? It largely comes down to our unique physiology and how our bodies process alcohol. Women generally have less body water than men of the same weight, which means alcohol becomes more concentrated in our system. On top of that, our stomachs produce less of the enzyme that breaks down alcohol before it even reaches the bloodstream. This combination means we absorb more alcohol and it takes longer to metabolize, leading to more prolonged exposure to the carcinogen acetaldehyde. This increased exposure, combined with alcohol’s tendency to disrupt our hormonal health, creates a perfect storm that elevates the risk for cancers of the breast, ovaries, and endometrium.
In addition to triggering these internal mechanisms, alcohol can increase cancer risk indirectly by making it easier for other harmful processes to take place.
Alcohol can act as a solvent, making it easier for carcinogenic chemicals — such as tobacco smoke — to enter our cells. It can also weaken our immune system, making it harder for us to fight off diseases, including cancer.
We’ve all heard it, right? That a glass of red wine with dinner is actually good for you, especially your heart. But this popular belief often glosses over a much more serious reality: the significant cancer risks tied to drinking any kind of alcohol. The truth is, when it comes to cancer, your body doesn't distinguish between a fancy Merlot and a cheap beer. The common denominator in all alcoholic drinks is ethanol, and that's where the trouble begins. All types of alcohol, whether it's wine, beer, or liquor, carry the same cancer risk because they all contain this compound.
So, what about drinking in moderation? Unfortunately, experts are clear that there is no safe amount of alcohol when it comes to cancer. Even a small amount increases your risk. While some studies have pointed to potential heart benefits from the antioxidants in red wine, these benefits simply don't outweigh the proven cancer risks. The more alcohol you consume, the higher your risk becomes. It's a straightforward relationship that puts the "healthy glass of wine" idea into a much different perspective, encouraging us to look at the complete picture of how alcohol affects our long-term health.
So how can we use this information to live healthier lives? For one, cutting back on alcohol or abstaining altogether can significantly reduce our risk.
Here are some additional changes that can make a big difference:
Together, we can navigate the journey to a healthier, happier life. Remember, every little step counts!
When it comes to alcohol and health, it helps to have a clear benchmark. Official guidelines from health organizations like the Centers for Disease Control and Prevention (CDC) provide a framework based on scientific evidence. These recommendations aren't about judgment; they're about giving you the information you need to make choices that align with your health goals. Understanding what experts consider moderate consumption is a crucial first step in evaluating your own habits. It allows you to see where you stand and decide what, if any, changes you’d like to make. Think of it as a map — it shows you the terrain so you can choose your path forward.
One of the biggest hurdles in tracking alcohol intake is knowing what a “standard drink” actually is. It’s easy to underestimate how much you’re consuming when drink sizes vary so much. According to the MD Anderson Cancer Center, one standard drink is defined as 12 ounces of beer, 5 ounces of wine, or 1.5 ounces of 80-proof liquor. That generous glass of wine you pour at home could easily count as two standard drinks. Being aware of these measurements is key to accurately assessing your consumption and understanding your risk. It’s the foundation of mindful drinking and helps you stay honest with yourself about your habits.
So, what do the experts recommend? The CDC advises that if you choose to drink, you do so in moderation. For women, this means one standard drink or less per day, and for men, it’s two standard drinks or less per day. It’s important to remember that these are upper limits for the days you do drink, not daily targets to aim for. The healthiest option is always to drink less. These guidelines are designed to help minimize health risks, including the risk of cancer. Sticking to them is a powerful way to protect your long-term well-being while still allowing yourself to enjoy a drink on occasion if you choose to.
The link between how much you drink and your cancer risk is direct and significant. It’s not just heavy drinking that poses a threat; even moderate amounts can increase your chances of developing certain cancers. According to the Canadian Cancer Society, consuming about 3.5 drinks a day can double or even triple your risk of cancers in the mouth, throat, and esophagus. The same amount increases the risk of colon and breast cancer by 1.5 times. This dose-response relationship is clear: the more you drink, the higher your risk. This knowledge is empowering because it puts the control back in your hands. Every drink you skip is a step toward lowering that risk.
If you're feeling concerned, here’s some good news: it’s never too late to make a positive change. When you stop drinking, your risk for alcohol-related cancers begins to decrease over time. While it may take many years for the risk to be fully removed, quitting is a significant and proactive step for your health. Your body has an incredible capacity for healing, and reducing its exposure to carcinogens like acetaldehyde gives it a chance to repair. This journey of mindful drinking or quitting entirely is one of the most impactful things you can do for your future self, and every day alcohol-free is a victory for your long-term health.
For anyone currently facing a cancer diagnosis or in recovery, the conversation around alcohol becomes even more critical. It’s essential to talk to your doctor about your alcohol use. Drinking can interfere with treatment, worsen side effects, and potentially increase the risk of developing new cancers. Your healthcare team can provide personalized advice based on your specific diagnosis, treatment plan, and overall health. This conversation is a vital part of your care, ensuring that your lifestyle choices support your recovery and help protect your health moving forward. Don't hesitate to bring it up; your medical team is there to support you in every aspect of your journey.
I've always heard that a glass of red wine is good for you. Is that not true when it comes to cancer? That's a common belief, but when we're talking about cancer risk, the type of alcohol doesn't matter. Whether it's wine, beer, or liquor, they all contain ethanol, which your body converts into a cancer-causing chemical. While some studies point to antioxidants in red wine for heart health, those benefits don't cancel out the proven cancer risk that comes with any alcoholic drink.
Does even light or moderate drinking really increase my cancer risk? Yes, unfortunately, the evidence is clear that even small amounts of alcohol can increase your risk for certain cancers. There isn't a "safe" threshold when it comes to cancer prevention. The relationship is straightforward: the more you drink over time, the higher your risk becomes. This is why understanding what a standard drink is and being mindful of your intake is so important.
Why is the cancer risk from alcohol higher for women? It really comes down to our physiology. Women tend to have less body water than men, which means alcohol becomes more concentrated in our systems. We also produce less of a key enzyme in our stomachs that breaks down alcohol. This combination leads to higher blood alcohol concentrations and longer exposure to its harmful byproducts, which, along with alcohol's effect on hormones like estrogen, elevates our risk.
What is the main way alcohol actually causes cancer? The primary culprit is a toxic chemical called acetaldehyde. When you drink alcohol, your body works to break it down, and acetaldehyde is the main byproduct of that process. This chemical is a known carcinogen that can directly damage the DNA in your cells and prevent your body from repairing that damage. Over time, this can lead to mutations that cause cells to grow uncontrollably.
If I cut back or stop drinking now, can I actually lower my risk? Absolutely. It's one of the most empowering things to know. While it can take time, your body has an amazing ability to heal. When you reduce or eliminate alcohol, you lower your exposure to its cancer-causing effects, and your risk for developing alcohol-related cancers begins to decrease. Every step you take toward drinking less is a positive move for your long-term health.

Scientists have established that alcohol consumption increases the risk of breast cancer through two mechanisms: elevated levels of certain hormones and potential DNA damage.
Although it isn’t a treatment for alcohol use disorder (AUD), the Reframe app can help you cut back on drinking gradually, with the science-backed knowledge to empower you 100% of the way. Our proven program has helped millions of people around the world drink less and live more. And we want to help you get there, too!
The Reframe app equips you with the knowledge and skills you need to not only survive drinking less, but to thrive while you navigate the journey. Our daily research-backed readings teach you the neuroscience of alcohol, and our in-app Toolkit provides the resources and activities you need to navigate each challenge.
You’ll meet millions of fellow Reframers in our 24/7 Forum chat and daily Zoom check-in meetings. Receive encouragement from people worldwide who know exactly what you’re going through! You’ll also have the opportunity to connect with our licensed Reframe coaches for more personalized guidance.
Plus, we’re always introducing new features to optimize your in-app experience. We recently launched our in-app chatbot, Melody, powered by the world’s most powerful AI technology. Melody is here to help as you adjust to a life with less (or no) alcohol.
And that’s not all! Every month, we launch fun challenges, like Dry/Damp January, Mental Health May, and Outdoorsy June. You won’t want to miss out on the chance to participate alongside fellow Reframers (or solo if that’s more your thing!).
The Reframe app is free for 7 days, so you don’t have anything to lose by trying it. Are you ready to feel empowered and discover life beyond alcohol? Then download our app today!
We all know someone who’s been affected by breast cancer — a family member, a coworker, or a friend of a friend. It's a topic that's never far from our minds. As many as 1 in 8 women will experience it at some point, and it accounts for over 12% of new cancer cases diagnosed around the globe every year. In the U.S. alone, there are currently around 4 million women with a history of breast cancer.
However, it's not all doom and gloom. The more we understand about breast cancer and its risk factors, the more empowered we are to take control of our health.
One connection that’s often overlooked is the link between breast cancer risk and alcohol. There's been a flurry of scientific research in this area in the last few decades, and we're here to make sense of it all.
Breast cancer (like all cancers) begins when cells in the breast start growing in an uncontrolled way. These rogue cells can band together to form a lump or tumor and might even spread to other parts of the body if left unchecked.
Breast cancer comes in two major types:
While the exact "why" behind many cancers is a mystery, certain factors make breast cancer more likely.
Breast cancer isn't about who you are or where you live — women all over the globe face it, and it's the leading cancer among women. However, with knowledge and support, we can face it head-on.
Catching breast cancer early makes a world of difference, and there are several ways to do so.
Because of its impact on women and families around the world, breast cancer awareness has become a global movement. Breast Cancer Awareness Month (BCAM), observed every October, was established in the United States in 1985 as a partnership between the pharmaceutical company AstraZeneca, which produced several breast cancer drugs, and various cancer charities and organizations.
The primary aim of this initiative was two-fold:
While Breast Cancer Awareness Month started in the mid-80s, the pink ribbon symbol for breast cancer awareness came onto the scene a few years later, when an activist named Charlotte Haley began making peach-colored ribbons in her home. She distributed the ribbons with cards that read, "The National Cancer Institute's annual budget is $1.8 billion, with only 5% going to cancer prevention. Help us wake up our legislators and America by wearing this ribbon."
In 1991, the Susan G. Komen Foundation first handed out pink ribbons at a New York City race for breast cancer survivors — an event that turned the pink ribbon into the symbol we all recognize today. By 1992, several major breast cancer charities had officially adopted it as the symbol for Breast Cancer Awareness Month.
From its beginnings in the United States, Breast Cancer Awareness Month rapidly gained traction around the world. Today, it’s more than just a month on the calendar — it’s a global movement. Advancements in medical science and the power of social media have expanded the scope and reach of the awareness campaigns. Personal stories of battles fought and won, tributes to those lost, and the unwavering commitment of organizations and advocates have helped humanize the cause.
Numerous countries worldwide now recognize October as a month dedicated to breast cancer awareness, research, fundraising, and community events. Here are just a few examples:

But what does an occasional glass of wine have to do with breast cancer? It's a valid question, and we've got some science-based answers.
Over the years, the evidence has become clear and strong: the more alcohol we consume, the higher our risk of breast cancer.
Recent research has brought more insight into this connection, with several studies worldwide confirming the link between alcohol and breast cancer. Scientists report that even light to moderate drinking — up to one drink per day — significantly increased the chances of developing the disease. This risk also appears to be cumulative: the more alcohol we drink over our lifetime, the higher our risk becomes.
When we drink, our bodies convert it into a chemical called acetaldehyde — a potent carcinogen that can damage our DNA and proteins, leading to cancerous changes in cells. While our liver enzymes further break down acetaldehyde into non-toxic substances, high levels of alcohol consumption can lead to a buildup of acetaldehyde, which the liver can't process quickly enough.
This buildup of acetaldehyde may play a crucial role in the development of cancer cells. Acetaldehyde can bind to proteins and DNA in cells, causing mutations that can lead to cancer. This DNA damage is cumulative: the more alcohol we consume over time, the greater the potential for harm and the increased risk of developing cancer.
Breast tissue is particularly sensitive to this process, which explains why the risk of breast cancer is especially high.
There's another angle to consider as well. Alcohol can increase levels of estrogen and other hormones associated with breast cancer. Let’s explore this connection in more detail.
Hormones are chemical messengers produced by our endocrine glands. They travel through our bloodstream, instructing tissues and organs on what to do in our bodies. Estrogen, a primary female sex hormone, plays a vital role in a woman's reproductive cycle and overall health.
It’s responsible for the growth and development of female sexual characteristics, including the breasts. Estrogen spikes during the menstrual cycle have been linked to breast cell proliferation. While this is a natural process, an overexposure or prolonged exposure to estrogen can increase the risk of breast cancer by increasing cell division and raising the chance of DNA mutations.
Many breast cancers are estrogen-receptor-positive: they have receptors for estrogen. When estrogen binds to these receptors, it can stimulate the cancer to grow. This is why hormone therapies that reduce the body's estrogen levels or block estrogen from binding to its receptors are often used to treat these types of breast cancer.
Alcohol can increase levels of estrogen in the body in different ways:
In breast cancers that are estrogen-receptor-positive, the presence of the hormone can also accelerate tumor growth. Since alcohol increases estrogen levels, it can indirectly promote the growth of these estrogen-sensitive tumors.
While estrogen is a primary concern, alcohol also affects other hormones that can indirectly influence breast cancer risk:
While all of this might sound alarming, let's put these findings in perspective. It's important to remember that while alcohol influences hormone levels, not everyone who drinks will develop breast cancer (just as not everyone who doesn’t drink is guaranteed to not get it). In the end, this is about risk — not certainty — and factors like genetics, overall health, and other lifestyle choices all play a role. Alcohol is just one piece of the puzzle.
Still, the research is clear: this is one puzzle piece we shouldn’t ignore! The good news is that this is also a piece we have some control over.
By understanding the connection between alcohol and breast cancer, we can balance our choices to maximize our health and enjoyment of life. When it comes to reducing our risk of breast cancer, so much power is in our hands. We might not be able to change our genes, but our lifestyle choices can have a big impact on our health. Let's explore what we actually can control.
By incorporating these steps into our routine, we're not just reducing our risk of breast cancer — we're also boosting our overall health, vitality, and well-being. It's all about making choices that respect and nurture our bodies.
All in all, the journey to reduce our risk of breast cancer is one of awareness, informed decisions, and empowerment. Despite how it feels at times, we’re not alone. We're part of a community, a collective of strong individuals making daily decisions to promote our health. Every small choice matters. Every step we take towards healthier habits, like reducing our alcohol intake, is a step towards reducing our breast cancer risk!
We all know someone who’s been affected by breast cancer — a family member, a coworker, or a friend of a friend. It's a topic that's never far from our minds. As many as 1 in 8 women will experience it at some point, and it accounts for over 12% of new cancer cases diagnosed around the globe every year. In the U.S. alone, there are currently around 4 million women with a history of breast cancer.
However, it's not all doom and gloom. The more we understand about breast cancer and its risk factors, the more empowered we are to take control of our health.
One connection that’s often overlooked is the link between breast cancer risk and alcohol. There's been a flurry of scientific research in this area in the last few decades, and we're here to make sense of it all.
Breast cancer (like all cancers) begins when cells in the breast start growing in an uncontrolled way. These rogue cells can band together to form a lump or tumor and might even spread to other parts of the body if left unchecked.
Breast cancer comes in two major types:
While the exact "why" behind many cancers is a mystery, certain factors make breast cancer more likely.
Breast cancer isn't about who you are or where you live — women all over the globe face it, and it's the leading cancer among women. However, with knowledge and support, we can face it head-on.
Catching breast cancer early makes a world of difference, and there are several ways to do so.
Because of its impact on women and families around the world, breast cancer awareness has become a global movement. Breast Cancer Awareness Month (BCAM), observed every October, was established in the United States in 1985 as a partnership between the pharmaceutical company AstraZeneca, which produced several breast cancer drugs, and various cancer charities and organizations.
The primary aim of this initiative was two-fold:
While Breast Cancer Awareness Month started in the mid-80s, the pink ribbon symbol for breast cancer awareness came onto the scene a few years later, when an activist named Charlotte Haley began making peach-colored ribbons in her home. She distributed the ribbons with cards that read, "The National Cancer Institute's annual budget is $1.8 billion, with only 5% going to cancer prevention. Help us wake up our legislators and America by wearing this ribbon."
In 1991, the Susan G. Komen Foundation first handed out pink ribbons at a New York City race for breast cancer survivors — an event that turned the pink ribbon into the symbol we all recognize today. By 1992, several major breast cancer charities had officially adopted it as the symbol for Breast Cancer Awareness Month.
From its beginnings in the United States, Breast Cancer Awareness Month rapidly gained traction around the world. Today, it’s more than just a month on the calendar — it’s a global movement. Advancements in medical science and the power of social media have expanded the scope and reach of the awareness campaigns. Personal stories of battles fought and won, tributes to those lost, and the unwavering commitment of organizations and advocates have helped humanize the cause.
Numerous countries worldwide now recognize October as a month dedicated to breast cancer awareness, research, fundraising, and community events. Here are just a few examples:

But what does an occasional glass of wine have to do with breast cancer? It's a valid question, and we've got some science-based answers.
Over the years, the evidence has become clear and strong: the more alcohol we consume, the higher our risk of breast cancer.
Recent research has brought more insight into this connection, with several studies worldwide confirming the link between alcohol and breast cancer. Scientists report that even light to moderate drinking — up to one drink per day — significantly increased the chances of developing the disease. This risk also appears to be cumulative: the more alcohol we drink over our lifetime, the higher our risk becomes.
When we drink, our bodies convert it into a chemical called acetaldehyde — a potent carcinogen that can damage our DNA and proteins, leading to cancerous changes in cells. While our liver enzymes further break down acetaldehyde into non-toxic substances, high levels of alcohol consumption can lead to a buildup of acetaldehyde, which the liver can't process quickly enough.
This buildup of acetaldehyde may play a crucial role in the development of cancer cells. Acetaldehyde can bind to proteins and DNA in cells, causing mutations that can lead to cancer. This DNA damage is cumulative: the more alcohol we consume over time, the greater the potential for harm and the increased risk of developing cancer.
Breast tissue is particularly sensitive to this process, which explains why the risk of breast cancer is especially high.
There's another angle to consider as well. Alcohol can increase levels of estrogen and other hormones associated with breast cancer. Let’s explore this connection in more detail.
Hormones are chemical messengers produced by our endocrine glands. They travel through our bloodstream, instructing tissues and organs on what to do in our bodies. Estrogen, a primary female sex hormone, plays a vital role in a woman's reproductive cycle and overall health.
It’s responsible for the growth and development of female sexual characteristics, including the breasts. Estrogen spikes during the menstrual cycle have been linked to breast cell proliferation. While this is a natural process, an overexposure or prolonged exposure to estrogen can increase the risk of breast cancer by increasing cell division and raising the chance of DNA mutations.
Many breast cancers are estrogen-receptor-positive: they have receptors for estrogen. When estrogen binds to these receptors, it can stimulate the cancer to grow. This is why hormone therapies that reduce the body's estrogen levels or block estrogen from binding to its receptors are often used to treat these types of breast cancer.
Alcohol can increase levels of estrogen in the body in different ways:
In breast cancers that are estrogen-receptor-positive, the presence of the hormone can also accelerate tumor growth. Since alcohol increases estrogen levels, it can indirectly promote the growth of these estrogen-sensitive tumors.
While estrogen is a primary concern, alcohol also affects other hormones that can indirectly influence breast cancer risk:
While all of this might sound alarming, let's put these findings in perspective. It's important to remember that while alcohol influences hormone levels, not everyone who drinks will develop breast cancer (just as not everyone who doesn’t drink is guaranteed to not get it). In the end, this is about risk — not certainty — and factors like genetics, overall health, and other lifestyle choices all play a role. Alcohol is just one piece of the puzzle.
Still, the research is clear: this is one puzzle piece we shouldn’t ignore! The good news is that this is also a piece we have some control over.
By understanding the connection between alcohol and breast cancer, we can balance our choices to maximize our health and enjoyment of life. When it comes to reducing our risk of breast cancer, so much power is in our hands. We might not be able to change our genes, but our lifestyle choices can have a big impact on our health. Let's explore what we actually can control.
By incorporating these steps into our routine, we're not just reducing our risk of breast cancer — we're also boosting our overall health, vitality, and well-being. It's all about making choices that respect and nurture our bodies.
All in all, the journey to reduce our risk of breast cancer is one of awareness, informed decisions, and empowerment. Despite how it feels at times, we’re not alone. We're part of a community, a collective of strong individuals making daily decisions to promote our health. Every small choice matters. Every step we take towards healthier habits, like reducing our alcohol intake, is a step towards reducing our breast cancer risk!

Alcohol poisoning brain damage is a real risk. Learn the signs, symptoms, and steps you can take to protect your brain and support safer drinking habits.
The Reframe app is here for you! We've already helped hundreds of thousands of people just like you examine their drinking habits and develop healthier routines. We would love to do the same for you!
Everyone has a different story, and our goal is to help you understand how your relationship with alcohol has affected your life. Once you join our vibrant community, you'll receive daily Readings to help you deal with all kinds of stressors. You’ll also have 24/7 access to our Forum chat. We're an eclectic, lively bunch from all corners of the globe, all tackling similar questions and challenges.
Best of all, you can try the Reframe app for a full 7 days, completely free! There's absolutely no risk and so much potential benefit! Think about finally getting back the mental clarity, energy, and happiness you deserve. We're here to help, cheering you on to live your best life. See you soon in the app!
Nobody heads out for a birthday celebration or happy hour with friends expecting the night to end in the ER. But sometimes, one drink turns into too many, and we don't see the dangerous path we're on. This path can lead to a medical emergency and, in severe cases, permanent alcohol poisoning brain damage. The risk of long-term alcohol brain damage is real, and it happens more often than you might think. Understanding how to respond when someone has had too much is critical—and it could save a life.
Let’s start from the beginning — how does alcohol affect the brain? Alcohol, a central nervous system depressant, slows down brain function and alters its structure. Prolonged heavy drinking can lead to brain shrinkage, specifically impacting regions associated with cognition and learning, and impairing neurogenesis.
Moreover, alcohol interferes with the neurotransmitters, the chemicals that transmit signals within the brain and throughout the body. This disruption can lead to changes in mood, behavior, and bodily functions. So what does alcohol do to your brain? Let’s find out!
When we talk about heavy drinking, we’re discussing a pattern that directly exposes the brain to a toxin. According to the Better Health Channel, “Alcohol is poisonous to the brain. It can also change how the body uses nutrients, affect blood flow to the brain, and stop the brain from getting enough vitamin B1 (thiamine), which is very important.” This isn't just a minor issue; a thiamine deficiency can lead to severe and permanent brain disorders, such as Wernicke-Korsakoff syndrome, which impacts memory and coordination. Essentially, excessive alcohol consumption starves the brain of critical nutrients it needs to function and repair itself, leading to significant and lasting damage over time.
Beyond the slow-burn damage from nutrient deficiencies, alcohol poses immediate, life-threatening risks. An overdose can overwhelm the body’s systems, and as the National Institute on Alcohol Abuse and Alcoholism (NIAAA) states, “Alcohol overdose can lead to permanent brain damage or death.” This often happens because high levels of alcohol can suppress the central nervous system so much that breathing becomes dangerously slow or stops altogether. This lack of oxygen, known as hypoxia, can cause irreversible brain damage within minutes. Seizures during severe intoxication can also lead to oxygen deprivation, further compounding the harm to brain cells.
While the brain is incredibly vulnerable, it’s not the only organ at risk from heavy alcohol use. The liver, which is responsible for metabolizing alcohol, can become fatty, inflamed (alcoholic hepatitis), and eventually scarred (cirrhosis), impairing its ability to function. The heart can weaken, leading to conditions like cardiomyopathy, where the heart muscle struggles to pump blood effectively. The pancreas is also at risk for pancreatitis, a painful and dangerous inflammation. As noted by Futures Recovery, “If the brain doesn't get enough oxygen during severe alcohol poisoning (for example, during seizures), it can cause permanent brain damage,” highlighting how a single event can have cascading effects throughout the body’s most critical systems.
It’s crucial to understand what alcohol poisoning actually is and how it happens. Sober.com defines it clearly: “Alcohol poisoning, also called alcohol overdose, is a very serious and sometimes deadly problem caused by drinking too much alcohol too quickly.” When you drink, your liver works to filter the alcohol out of your blood. However, it can only process about one standard drink per hour. If you drink faster than your liver can work, your blood alcohol concentration (BAC) rises. This is the point where the toxic effects of alcohol begin to overwhelm the brain’s control over basic life-support functions like breathing, heart rate, and temperature regulation.
What many people don’t realize is that your BAC can continue to rise even after you’ve stopped drinking. Alcohol in the stomach and intestines continues to enter the bloodstream, meaning a dangerous situation can become critical even after a person has passed out. This is why it’s never safe to just “let someone sleep it off.” Understanding your own limits and practicing mindful drinking by pacing yourself, staying hydrated, and eating food can help prevent your body from becoming overwhelmed. It’s about being aware of not just what you drink, but how you drink it.
The most common path to alcohol poisoning is through binge drinking. This isn’t about having a few drinks over an entire evening; it’s about consuming a large amount in a very short period. Sober.com defines binge drinking as a pattern that brings a person’s BAC to 0.08% or higher, which typically happens after “4 or more drinks for women, or 5 or more for men, within 2 hours.” This rapid intake floods the system, giving the liver no chance to keep up. The result is a sharp spike in BAC that can quickly reach dangerous levels, leading to impaired judgment, loss of coordination, and, in severe cases, a complete shutdown of vital bodily functions.
Part of the reason people accidentally binge drink is a misunderstanding of what constitutes a “standard” drink. The NIAAA clarifies that in the U.S., “one standard drink has 0.6 fluid ounces or 14 grams of pure alcohol.” This translates to 12 ounces of regular beer (at 5% ABV), 5 ounces of wine (at 12% ABV), or 1.5 ounces of distilled spirits (at 40% ABV, or 80 proof). Think about the drinks you’re often served—a heavy-handed pour of wine, a pint of high-gravity craft beer, or a mixed drink with multiple shots. These often contain far more than one standard drink, making it easy to lose track and consume a dangerous amount of alcohol much faster than you realize.
While anyone can be at risk for alcohol poisoning, certain behaviors dramatically increase the danger. As Futures Recovery points out, “Binge drinking is the main cause. This means drinking a lot of alcohol in a short time.” This single factor—speed of consumption—is the most significant contributor. However, other elements play a role as well. Your body size and weight, whether you’ve eaten recently, your overall health, and your individual tolerance level all influence how quickly your BAC rises. Someone who rarely drinks may be at higher risk than a regular drinker, but even those with a high tolerance can easily cross the line into overdose territory during a binge.
Combining alcohol with other substances is one of the most dangerous things you can do. The Better Health Channel warns, “Mixing alcohol with other drugs (like opioids) is very dangerous and greatly increases the risk.” Alcohol is a central nervous system depressant, and when you mix it with other depressants—such as opioids, sedatives, or even some over-the-counter cold medications—you create a synergistic effect. This means the combined impact is far greater than the sum of its parts. This combination can severely slow breathing and heart rate, leading to respiratory failure, coma, and death. It’s a risk that is simply not worth taking.
Your personal biology and history also contribute to your risk. The Better Health Channel notes, “People who drink heavily for a long time are most at risk. However, even binge drinking can cause brain damage in just a few years.” Factors like age, gender, genetics, and pre-existing health conditions can affect how your body metabolizes alcohol. For example, women tend to have a higher BAC than men after consuming the same amount of alcohol. Understanding how these factors apply to you is key to making safer choices. Using a tool like a Blood Alcohol Content (BAC) calculator can provide a rough estimate, but it’s always wisest to err on the side of caution.
How does alcohol poisoning fit into all this? Consuming alcohol faster than our liver can process it overloads our system, causing a rapid increase in our blood alcohol concentration (BAC). A BAC that’s too high can lead to alcohol poisoning.
BAC levels higher than 0.3% can potentially be life-threatening, causing breathing difficulties and seizures. The effects of alcohol on the brain during binge drinking can be fatal. Although you might not be thinking about brain damage from alcohol when you sit down at the bar, things can take a dark turn if you aren’t careful.
During an episode of alcohol poisoning, the high level of alcohol depresses the nervous system so much that it can't perform its regular functions, such as controlling heart rate and breathing. This acute stress can trigger inflammation and oxidative stress in the brain — the sudden spike can impair the brain's ability to function properly, leading to unconsciousness, respiratory failure, and even death.
For this reason, alcohol poisoning is not a mere hangover — it's a medical emergency! In the most severe cases, it can result in alcohol-related brain damage (ARBD), characterized by cognitive deficits, impaired executive function, and difficulty with balance.
Knowing the signs of alcohol poisoning can be the difference between life and death. It’s not just about being very drunk; it’s a serious medical state. According to the National Institute on Alcohol Abuse and Alcoholism (NIAAA), key symptoms include mental confusion, vomiting, and seizures. You might also notice someone has trouble staying conscious, very slow breathing (fewer than eight breaths a minute), a slow heart rate, or clammy skin. Another critical sign is a dulled gag reflex, which is dangerous because it can lead to choking on vomit. An extremely low body temperature, which can cause the skin to look pale or bluish, is also a major red flag.
If you suspect someone has alcohol poisoning, treat it as the emergency it is. The most important step is to call 911 immediately. Don't wait for all the symptoms to appear or second-guess yourself. While you wait for medical help to arrive, try to keep the person awake and sitting up. If they must lie down, turn them onto their side to prevent them from choking if they vomit — this is known as the recovery position. Never leave them alone. Having someone there to monitor their breathing and consciousness can provide crucial information to the paramedics when they arrive.
There are many myths about how to sober someone up, and trying them can make a dangerous situation even worse. The NIAAA warns against common but ineffective methods. Do not give the person coffee; caffeine can dehydrate them further. Do not put them in a cold shower, as this can increase the risk of hypothermia, especially since their body temperature may already be dangerously low. Trying to make them walk it off is also a bad idea, as it can lead to falls and injuries. None of these "remedies" will lower a person's BAC, and they can create additional complications for someone in a vulnerable state.
One of the most dangerous mistakes you can make is assuming an unconscious person will simply "sleep it off." Even after someone stops drinking and passes out, their body continues to absorb alcohol from their stomach into their bloodstream. This means their BAC can keep rising to a fatal level. An unconscious person is also at high risk of choking on their own vomit because their gag reflex is suppressed. Never leave an unconscious person alone. Stay with them and get medical help right away.
So, what’s actually happening in the body during an overdose? Alcohol poisoning occurs when you drink a large amount of alcohol in a short period, overwhelming your liver's ability to process it. This causes your blood alcohol content (BAC) to spike to dangerous levels. Alcohol is a depressant, meaning it slows down brain functions. When your BAC gets too high, it can start to shut down the critical areas of your brain that control essential life-sustaining functions like breathing, heart rate, and body temperature. This isn't just a more intense version of being drunk; it's a life-threatening medical event that can cause permanent brain damage or death.
Understanding how BAC works is key to understanding the risk of an overdose. When you drink, alcohol is absorbed into your bloodstream through your stomach and small intestine. As the NIAAA explains, this process continues even after you’ve stopped drinking. This is why someone can seem fine one moment and be in serious trouble the next. Their BAC can continue to climb long after their last sip, especially if they drank a lot very quickly. If you're curious about how different factors affect your own BAC, you can use a Blood Alcohol Content (BAC) calculator to get a better sense of how your body processes alcohol.
Alcohol poisoning progresses through distinct stages as BAC levels rise. At a BAC of .11 to .15, the body often tries to expel the toxin, leading to vomiting. As the BAC climbs to between .17 and .30, a person may experience a blackout, where the brain temporarily stops recording memories. This is a sign of severe impairment. The most dangerous stage occurs when BAC reaches .31 or higher. At this point, the body’s vital functions can shut down, leading to a coma or even death. Recognizing these escalating signs is crucial for intervening before it’s too late.
When someone is hospitalized for alcohol poisoning, they receive immediate medical care to manage their symptoms and prevent long-term damage. This isn't something that can be treated at home. Medical professionals will carefully monitor their vital signs, including their heart rate and breathing. They might provide oxygen through a mask or insert a tube to help with breathing. An IV is often used to deliver fluids, which helps prevent dehydration and flush toxins from the body. They may also administer vitamins and glucose to prevent other serious complications associated with alcohol poisoning. In some cases, they may even pump the stomach to remove any unabsorbed alcohol.
If detected early, ARBD can be partially reversed with abstinence or a significant reduction in alcohol intake. Our brains are incredibly resilient: research has shown that after a period of abstinence, some damage can be reversed, and cognitive function can improve.
However, persistent episodes of alcohol poisoning can potentially cause brain damage to be permanent, eventually leading to Wernicke-Korsakoff syndrome, a severe form of ARBD.
Wernicke-Korsakoff syndrome comprises two separate conditions: Wernicke's encephalopathy and Korsakoff's psychosis. Wernicke's encephalopathy is a short-term but severe condition caused by a lack of vitamin B1 (thiamine) commonly seen in heavy drinkers. It is characterized by mental confusion, oculomotor disturbances (problems with eye movements), and difficulty with muscle coordination. If left untreated, this condition can lead to irreversible brain damage and even death.
If not treated immediately, it can lead to Korsakoff's psychosis, a long-term condition marked by learning and memory problems. While people with this condition may be able to recall events from long ago, they often struggle with new information or recent memories. They might also experience hallucinations or make up events to fill in memory gaps, a phenomenon known as confabulation.
Unfortunately, there's no specific cure for WKS. However, thiamine can be administered to prevent further deterioration of the brain, and in some cases, it may reverse some of the symptoms of Wernicke's encephalopathy and brain damage from alcohol.
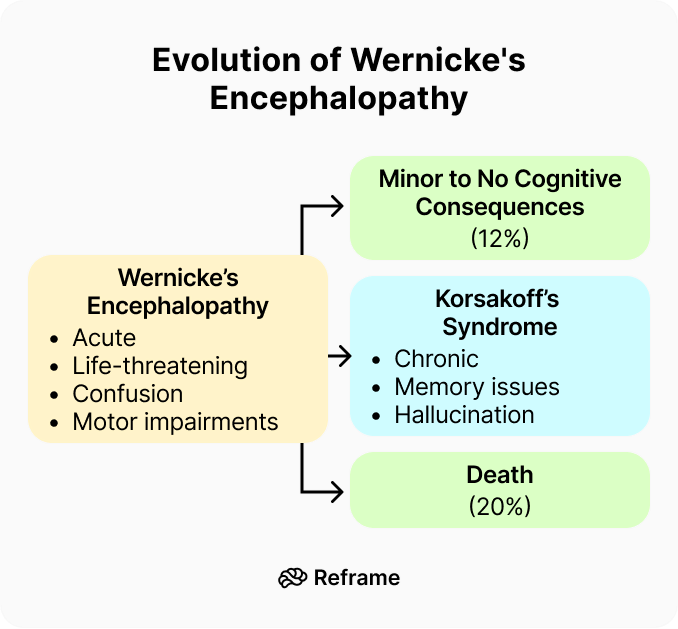
Alcohol-related brain damage, or ARBD, isn't a single condition but an umbrella term for the harm that can happen to the brain from long-term heavy drinking. It’s a direct result of alcohol's toxic effects on brain cells, often worsened by the nutritional gaps that can come with heavy alcohol use. Unlike other forms of dementia, the progression of ARBD can often be stopped — and sometimes even partially reversed — if a person stops drinking and gets the right support. This potential for recovery is a powerful motivator and makes catching the signs early absolutely critical for protecting your long-term health.
When we think of brain damage, memory loss is usually the first thing that comes to mind. But with ARBD, the symptoms are much broader and can impact your entire life. It can affect your ability to think clearly, make sound decisions, and plan your day. According to the Alzheimer's Society, you might find it hard to focus on tasks, feel unusually irritable or sad, or struggle with balance and coordination. Forgetting recent conversations, having trouble with planning, and experiencing sudden mood swings are all common signs. It’s a condition that affects your cognitive and physical well-being, not just your ability to recall information.
As we touched on earlier, one of the most severe forms of ARBD is Wernicke-Korsakoff syndrome (WKS). This isn't just one disease, but two distinct stages that are linked. First comes Wernicke's encephalopathy, an acute condition caused by a severe deficiency of thiamine (vitamin B1). This can lead to confusion, vision problems, and a loss of muscle coordination. If it’s not treated right away with high-dose thiamine, it can progress to Korsakoff's syndrome, a chronic and more permanent condition defined by severe short-term memory loss and difficulty forming new memories.
While any pattern of heavy, long-term drinking increases the risk of ARBD, some people are more vulnerable than others. It’s not just about how much you drink on a single occasion, but the cumulative effect of alcohol over months and years. Factors like your genetics, general health, and nutrition also play a significant role in how your body and brain respond to alcohol. Understanding the risk factors can help you recognize the warning signs in yourself or a loved one before the damage becomes more serious.
The numbers might be higher than you think. Research suggests that about one in three people who are dependent on alcohol show some signs of ARBD. The risk starts to climb for anyone regularly drinking 25 or more units per week — that’s equivalent to about eight pints of strong beer or just over two bottles of wine spread across the week. Consistent drinking above these levels can begin to impact your thinking skills and memory over time. It’s a stark reminder that what might feel like a normal habit can have serious long-term consequences for your brain health.
One of the most surprising things about ARBD is the age at which it typically appears. While we often associate dementia with older age, ARBD usually develops in people between 40 and 60. This is significantly younger than the typical onset for conditions like Alzheimer's. It tends to affect more men than women, largely because, historically, men have had higher rates of heavy drinking. Recognizing that ARBD can affect people in the prime of their lives underscores the importance of addressing drinking habits early on to protect your future.
Let's be clear: not every person who enjoys an occasional drink is destined for brain damage. It's all about understanding our limits and forming habits that ensure we drink responsibly. Here are five ways to do just that:
We live in a world where alcohol is often at the heart of social events. We don’t want to miss out on the fun of socializing and spending time with people we love … but we need to look after our health and to make sure we're not veering into dangerous territory. Does alcohol cause brain damage? Yes, but with the right decisions, we can stay safe. No alcohol poisoning or potential brain damage for us! Armed with knowledge, and by practicing responsible drinking habits, we can be part of the fun while socializing safely.
If you're worried about the impact alcohol is having on your brain, the first and most important step is to talk to a healthcare professional. While it can be scary to think about, there’s some good news. If it’s caught early, some alcohol-related brain damage can be reversed by stopping or significantly reducing your drinking. Our brains have an amazing capacity for healing; research shows that after a period of abstinence, some cognitive functions can improve. A doctor can help you create a safe plan to cut back and can also check for common nutritional deficiencies, like a lack of thiamine (vitamin B1), which can contribute to brain-related issues.
For those who drink heavily and consistently, the stakes are higher. Repeated episodes of alcohol poisoning can lead to permanent brain damage and may result in severe conditions like Wernicke-Korsakoff syndrome. This is why professional medical advice is not just helpful—it's critical. If you have a physical dependence on alcohol, quitting abruptly without medical supervision can be dangerous and lead to severe withdrawal symptoms. A doctor can provide the support and resources needed to manage withdrawal safely, setting you on a path toward recovery without risking your health further. Please don't try to go it alone.
If you or a loved one is dealing with ARBD, recovery is centered on a few key strategies. The most critical action is to stop drinking alcohol, which halts further damage and gives the brain a chance to heal. Alongside this, nutrition plays a huge role. As mentioned, many heavy drinkers are deficient in thiamine, which can cause severe neurological problems like Wernicke's encephalopathy. A doctor will often recommend thiamine supplements and a balanced diet rich in vitamins and minerals. Engaging in cognitive exercises, staying physically active, and maintaining a structured daily routine can also support brain function and help rebuild neural pathways.
Protecting your brain doesn't have to be an all-or-nothing battle. It’s really about understanding your personal limits and creating habits that support responsible drinking. This shift in mindset is powerful because it puts you back in control. Instead of focusing on what you’re giving up, you can focus on what you’re gaining: better health, clearer thinking, and more energy. The key is to start small. You don’t have to overhaul your entire life overnight. Begin by simply becoming more aware of your patterns. How much are you really drinking in a week? How does it make you feel the next day?
Once you have a clearer picture, you can set realistic goals. Maybe it’s committing to two alcohol-free days a week or deciding you’ll have only one drink at your next social gathering. Tools and apps designed for habit change, like Reframe, can be incredibly helpful for tracking your progress and providing support when you need it. Exploring the world of non-alcoholic cocktails or finding new hobbies that don’t revolve around drinking can also make the process feel less like a sacrifice and more like an exciting new chapter. You can find answers to common questions about this process in our FAQ section.
A great way to build healthier habits is to practice mindful drinking. This just means being more present and intentional with your choices around alcohol. It’s about asking yourself *why* you want a drink instead of reaching for one automatically. A simple mindful technique is to always eat a meal before you drink. Having food in your stomach slows the absorption of alcohol, giving your body more time to process it. Other practices include sipping your drink slowly to savor it, alternating each alcoholic beverage with a glass of water, and pausing before you get a refill to check in with how you’re feeling.
What’s the difference between being really drunk and having alcohol poisoning? Think of it this way: being drunk affects your coordination, judgment, and mood. Alcohol poisoning is a medical emergency where the amount of alcohol in your bloodstream is so high that it starts to shut down the parts of your brain that control basic life-support functions. If you see someone who is confused, vomiting, breathing very slowly, or can't be woken up, it's no longer about being drunk—it's a potential overdose that requires an immediate 911 call.
Can just one night of heavy drinking cause permanent brain damage? A single episode of severe alcohol poisoning can cause permanent brain damage, but not in the way you might think. The immediate danger comes from the body being deprived of oxygen, either from breathing that slows or stops, or from seizures. This lack of oxygen can harm brain cells. The more gradual brain damage, often called ARBD, typically develops from a pattern of heavy drinking over many years.
If someone passes out from drinking, isn't it best to just let them sleep it off? This is one of the most dangerous myths about alcohol. A person's blood alcohol level can continue to rise even after they've stopped drinking and passed out. This means they can go from being unconscious to having a fatal overdose while they're "sleeping." They are also at serious risk of choking if they vomit, as their gag reflex is suppressed. An unconscious person needs monitoring and immediate medical help.
Is brain damage from alcohol always permanent? Not always. The brain has a remarkable ability to heal. When someone stops drinking, especially if the damage is caught early, they can often see improvements in their cognitive function and memory. The key is to stop the exposure to alcohol to prevent further harm and give the brain a chance to recover. However, in very severe and long-term cases, such as Wernicke-Korsakoff syndrome, the damage can be lasting.
How do I know if I’m binge drinking if I don’t feel that drunk? Binge drinking is defined by the amount of alcohol consumed in a short time, not by how you feel. It's typically defined as having four or more drinks for women, or five or more for men, within about two hours. It's easy to hit this number without realizing it, especially since many cocktails, glasses of wine, or craft beers contain more than one "standard" serving of alcohol. It’s about the math, not the buzz.
Nobody heads out for a birthday celebration or happy hour with friends expecting the night to end in the ER. But sometimes, one drink turns into too many, and we don't see the dangerous path we're on. This path can lead to a medical emergency and, in severe cases, permanent alcohol poisoning brain damage. The risk of long-term alcohol brain damage is real, and it happens more often than you might think. Understanding how to respond when someone has had too much is critical—and it could save a life.
Let’s start from the beginning — how does alcohol affect the brain? Alcohol, a central nervous system depressant, slows down brain function and alters its structure. Prolonged heavy drinking can lead to brain shrinkage, specifically impacting regions associated with cognition and learning, and impairing neurogenesis.
Moreover, alcohol interferes with the neurotransmitters, the chemicals that transmit signals within the brain and throughout the body. This disruption can lead to changes in mood, behavior, and bodily functions. So what does alcohol do to your brain? Let’s find out!
When we talk about heavy drinking, we’re discussing a pattern that directly exposes the brain to a toxin. According to the Better Health Channel, “Alcohol is poisonous to the brain. It can also change how the body uses nutrients, affect blood flow to the brain, and stop the brain from getting enough vitamin B1 (thiamine), which is very important.” This isn't just a minor issue; a thiamine deficiency can lead to severe and permanent brain disorders, such as Wernicke-Korsakoff syndrome, which impacts memory and coordination. Essentially, excessive alcohol consumption starves the brain of critical nutrients it needs to function and repair itself, leading to significant and lasting damage over time.
Beyond the slow-burn damage from nutrient deficiencies, alcohol poses immediate, life-threatening risks. An overdose can overwhelm the body’s systems, and as the National Institute on Alcohol Abuse and Alcoholism (NIAAA) states, “Alcohol overdose can lead to permanent brain damage or death.” This often happens because high levels of alcohol can suppress the central nervous system so much that breathing becomes dangerously slow or stops altogether. This lack of oxygen, known as hypoxia, can cause irreversible brain damage within minutes. Seizures during severe intoxication can also lead to oxygen deprivation, further compounding the harm to brain cells.
While the brain is incredibly vulnerable, it’s not the only organ at risk from heavy alcohol use. The liver, which is responsible for metabolizing alcohol, can become fatty, inflamed (alcoholic hepatitis), and eventually scarred (cirrhosis), impairing its ability to function. The heart can weaken, leading to conditions like cardiomyopathy, where the heart muscle struggles to pump blood effectively. The pancreas is also at risk for pancreatitis, a painful and dangerous inflammation. As noted by Futures Recovery, “If the brain doesn't get enough oxygen during severe alcohol poisoning (for example, during seizures), it can cause permanent brain damage,” highlighting how a single event can have cascading effects throughout the body’s most critical systems.
It’s crucial to understand what alcohol poisoning actually is and how it happens. Sober.com defines it clearly: “Alcohol poisoning, also called alcohol overdose, is a very serious and sometimes deadly problem caused by drinking too much alcohol too quickly.” When you drink, your liver works to filter the alcohol out of your blood. However, it can only process about one standard drink per hour. If you drink faster than your liver can work, your blood alcohol concentration (BAC) rises. This is the point where the toxic effects of alcohol begin to overwhelm the brain’s control over basic life-support functions like breathing, heart rate, and temperature regulation.
What many people don’t realize is that your BAC can continue to rise even after you’ve stopped drinking. Alcohol in the stomach and intestines continues to enter the bloodstream, meaning a dangerous situation can become critical even after a person has passed out. This is why it’s never safe to just “let someone sleep it off.” Understanding your own limits and practicing mindful drinking by pacing yourself, staying hydrated, and eating food can help prevent your body from becoming overwhelmed. It’s about being aware of not just what you drink, but how you drink it.
The most common path to alcohol poisoning is through binge drinking. This isn’t about having a few drinks over an entire evening; it’s about consuming a large amount in a very short period. Sober.com defines binge drinking as a pattern that brings a person’s BAC to 0.08% or higher, which typically happens after “4 or more drinks for women, or 5 or more for men, within 2 hours.” This rapid intake floods the system, giving the liver no chance to keep up. The result is a sharp spike in BAC that can quickly reach dangerous levels, leading to impaired judgment, loss of coordination, and, in severe cases, a complete shutdown of vital bodily functions.
Part of the reason people accidentally binge drink is a misunderstanding of what constitutes a “standard” drink. The NIAAA clarifies that in the U.S., “one standard drink has 0.6 fluid ounces or 14 grams of pure alcohol.” This translates to 12 ounces of regular beer (at 5% ABV), 5 ounces of wine (at 12% ABV), or 1.5 ounces of distilled spirits (at 40% ABV, or 80 proof). Think about the drinks you’re often served—a heavy-handed pour of wine, a pint of high-gravity craft beer, or a mixed drink with multiple shots. These often contain far more than one standard drink, making it easy to lose track and consume a dangerous amount of alcohol much faster than you realize.
While anyone can be at risk for alcohol poisoning, certain behaviors dramatically increase the danger. As Futures Recovery points out, “Binge drinking is the main cause. This means drinking a lot of alcohol in a short time.” This single factor—speed of consumption—is the most significant contributor. However, other elements play a role as well. Your body size and weight, whether you’ve eaten recently, your overall health, and your individual tolerance level all influence how quickly your BAC rises. Someone who rarely drinks may be at higher risk than a regular drinker, but even those with a high tolerance can easily cross the line into overdose territory during a binge.
Combining alcohol with other substances is one of the most dangerous things you can do. The Better Health Channel warns, “Mixing alcohol with other drugs (like opioids) is very dangerous and greatly increases the risk.” Alcohol is a central nervous system depressant, and when you mix it with other depressants—such as opioids, sedatives, or even some over-the-counter cold medications—you create a synergistic effect. This means the combined impact is far greater than the sum of its parts. This combination can severely slow breathing and heart rate, leading to respiratory failure, coma, and death. It’s a risk that is simply not worth taking.
Your personal biology and history also contribute to your risk. The Better Health Channel notes, “People who drink heavily for a long time are most at risk. However, even binge drinking can cause brain damage in just a few years.” Factors like age, gender, genetics, and pre-existing health conditions can affect how your body metabolizes alcohol. For example, women tend to have a higher BAC than men after consuming the same amount of alcohol. Understanding how these factors apply to you is key to making safer choices. Using a tool like a Blood Alcohol Content (BAC) calculator can provide a rough estimate, but it’s always wisest to err on the side of caution.
How does alcohol poisoning fit into all this? Consuming alcohol faster than our liver can process it overloads our system, causing a rapid increase in our blood alcohol concentration (BAC). A BAC that’s too high can lead to alcohol poisoning.
BAC levels higher than 0.3% can potentially be life-threatening, causing breathing difficulties and seizures. The effects of alcohol on the brain during binge drinking can be fatal. Although you might not be thinking about brain damage from alcohol when you sit down at the bar, things can take a dark turn if you aren’t careful.
During an episode of alcohol poisoning, the high level of alcohol depresses the nervous system so much that it can't perform its regular functions, such as controlling heart rate and breathing. This acute stress can trigger inflammation and oxidative stress in the brain — the sudden spike can impair the brain's ability to function properly, leading to unconsciousness, respiratory failure, and even death.
For this reason, alcohol poisoning is not a mere hangover — it's a medical emergency! In the most severe cases, it can result in alcohol-related brain damage (ARBD), characterized by cognitive deficits, impaired executive function, and difficulty with balance.
Knowing the signs of alcohol poisoning can be the difference between life and death. It’s not just about being very drunk; it’s a serious medical state. According to the National Institute on Alcohol Abuse and Alcoholism (NIAAA), key symptoms include mental confusion, vomiting, and seizures. You might also notice someone has trouble staying conscious, very slow breathing (fewer than eight breaths a minute), a slow heart rate, or clammy skin. Another critical sign is a dulled gag reflex, which is dangerous because it can lead to choking on vomit. An extremely low body temperature, which can cause the skin to look pale or bluish, is also a major red flag.
If you suspect someone has alcohol poisoning, treat it as the emergency it is. The most important step is to call 911 immediately. Don't wait for all the symptoms to appear or second-guess yourself. While you wait for medical help to arrive, try to keep the person awake and sitting up. If they must lie down, turn them onto their side to prevent them from choking if they vomit — this is known as the recovery position. Never leave them alone. Having someone there to monitor their breathing and consciousness can provide crucial information to the paramedics when they arrive.
There are many myths about how to sober someone up, and trying them can make a dangerous situation even worse. The NIAAA warns against common but ineffective methods. Do not give the person coffee; caffeine can dehydrate them further. Do not put them in a cold shower, as this can increase the risk of hypothermia, especially since their body temperature may already be dangerously low. Trying to make them walk it off is also a bad idea, as it can lead to falls and injuries. None of these "remedies" will lower a person's BAC, and they can create additional complications for someone in a vulnerable state.
One of the most dangerous mistakes you can make is assuming an unconscious person will simply "sleep it off." Even after someone stops drinking and passes out, their body continues to absorb alcohol from their stomach into their bloodstream. This means their BAC can keep rising to a fatal level. An unconscious person is also at high risk of choking on their own vomit because their gag reflex is suppressed. Never leave an unconscious person alone. Stay with them and get medical help right away.
So, what’s actually happening in the body during an overdose? Alcohol poisoning occurs when you drink a large amount of alcohol in a short period, overwhelming your liver's ability to process it. This causes your blood alcohol content (BAC) to spike to dangerous levels. Alcohol is a depressant, meaning it slows down brain functions. When your BAC gets too high, it can start to shut down the critical areas of your brain that control essential life-sustaining functions like breathing, heart rate, and body temperature. This isn't just a more intense version of being drunk; it's a life-threatening medical event that can cause permanent brain damage or death.
Understanding how BAC works is key to understanding the risk of an overdose. When you drink, alcohol is absorbed into your bloodstream through your stomach and small intestine. As the NIAAA explains, this process continues even after you’ve stopped drinking. This is why someone can seem fine one moment and be in serious trouble the next. Their BAC can continue to climb long after their last sip, especially if they drank a lot very quickly. If you're curious about how different factors affect your own BAC, you can use a Blood Alcohol Content (BAC) calculator to get a better sense of how your body processes alcohol.
Alcohol poisoning progresses through distinct stages as BAC levels rise. At a BAC of .11 to .15, the body often tries to expel the toxin, leading to vomiting. As the BAC climbs to between .17 and .30, a person may experience a blackout, where the brain temporarily stops recording memories. This is a sign of severe impairment. The most dangerous stage occurs when BAC reaches .31 or higher. At this point, the body’s vital functions can shut down, leading to a coma or even death. Recognizing these escalating signs is crucial for intervening before it’s too late.
When someone is hospitalized for alcohol poisoning, they receive immediate medical care to manage their symptoms and prevent long-term damage. This isn't something that can be treated at home. Medical professionals will carefully monitor their vital signs, including their heart rate and breathing. They might provide oxygen through a mask or insert a tube to help with breathing. An IV is often used to deliver fluids, which helps prevent dehydration and flush toxins from the body. They may also administer vitamins and glucose to prevent other serious complications associated with alcohol poisoning. In some cases, they may even pump the stomach to remove any unabsorbed alcohol.
If detected early, ARBD can be partially reversed with abstinence or a significant reduction in alcohol intake. Our brains are incredibly resilient: research has shown that after a period of abstinence, some damage can be reversed, and cognitive function can improve.
However, persistent episodes of alcohol poisoning can potentially cause brain damage to be permanent, eventually leading to Wernicke-Korsakoff syndrome, a severe form of ARBD.
Wernicke-Korsakoff syndrome comprises two separate conditions: Wernicke's encephalopathy and Korsakoff's psychosis. Wernicke's encephalopathy is a short-term but severe condition caused by a lack of vitamin B1 (thiamine) commonly seen in heavy drinkers. It is characterized by mental confusion, oculomotor disturbances (problems with eye movements), and difficulty with muscle coordination. If left untreated, this condition can lead to irreversible brain damage and even death.
If not treated immediately, it can lead to Korsakoff's psychosis, a long-term condition marked by learning and memory problems. While people with this condition may be able to recall events from long ago, they often struggle with new information or recent memories. They might also experience hallucinations or make up events to fill in memory gaps, a phenomenon known as confabulation.
Unfortunately, there's no specific cure for WKS. However, thiamine can be administered to prevent further deterioration of the brain, and in some cases, it may reverse some of the symptoms of Wernicke's encephalopathy and brain damage from alcohol.

Alcohol-related brain damage, or ARBD, isn't a single condition but an umbrella term for the harm that can happen to the brain from long-term heavy drinking. It’s a direct result of alcohol's toxic effects on brain cells, often worsened by the nutritional gaps that can come with heavy alcohol use. Unlike other forms of dementia, the progression of ARBD can often be stopped — and sometimes even partially reversed — if a person stops drinking and gets the right support. This potential for recovery is a powerful motivator and makes catching the signs early absolutely critical for protecting your long-term health.
When we think of brain damage, memory loss is usually the first thing that comes to mind. But with ARBD, the symptoms are much broader and can impact your entire life. It can affect your ability to think clearly, make sound decisions, and plan your day. According to the Alzheimer's Society, you might find it hard to focus on tasks, feel unusually irritable or sad, or struggle with balance and coordination. Forgetting recent conversations, having trouble with planning, and experiencing sudden mood swings are all common signs. It’s a condition that affects your cognitive and physical well-being, not just your ability to recall information.
As we touched on earlier, one of the most severe forms of ARBD is Wernicke-Korsakoff syndrome (WKS). This isn't just one disease, but two distinct stages that are linked. First comes Wernicke's encephalopathy, an acute condition caused by a severe deficiency of thiamine (vitamin B1). This can lead to confusion, vision problems, and a loss of muscle coordination. If it’s not treated right away with high-dose thiamine, it can progress to Korsakoff's syndrome, a chronic and more permanent condition defined by severe short-term memory loss and difficulty forming new memories.
While any pattern of heavy, long-term drinking increases the risk of ARBD, some people are more vulnerable than others. It’s not just about how much you drink on a single occasion, but the cumulative effect of alcohol over months and years. Factors like your genetics, general health, and nutrition also play a significant role in how your body and brain respond to alcohol. Understanding the risk factors can help you recognize the warning signs in yourself or a loved one before the damage becomes more serious.
The numbers might be higher than you think. Research suggests that about one in three people who are dependent on alcohol show some signs of ARBD. The risk starts to climb for anyone regularly drinking 25 or more units per week — that’s equivalent to about eight pints of strong beer or just over two bottles of wine spread across the week. Consistent drinking above these levels can begin to impact your thinking skills and memory over time. It’s a stark reminder that what might feel like a normal habit can have serious long-term consequences for your brain health.
One of the most surprising things about ARBD is the age at which it typically appears. While we often associate dementia with older age, ARBD usually develops in people between 40 and 60. This is significantly younger than the typical onset for conditions like Alzheimer's. It tends to affect more men than women, largely because, historically, men have had higher rates of heavy drinking. Recognizing that ARBD can affect people in the prime of their lives underscores the importance of addressing drinking habits early on to protect your future.
Let's be clear: not every person who enjoys an occasional drink is destined for brain damage. It's all about understanding our limits and forming habits that ensure we drink responsibly. Here are five ways to do just that:
We live in a world where alcohol is often at the heart of social events. We don’t want to miss out on the fun of socializing and spending time with people we love … but we need to look after our health and to make sure we're not veering into dangerous territory. Does alcohol cause brain damage? Yes, but with the right decisions, we can stay safe. No alcohol poisoning or potential brain damage for us! Armed with knowledge, and by practicing responsible drinking habits, we can be part of the fun while socializing safely.
If you're worried about the impact alcohol is having on your brain, the first and most important step is to talk to a healthcare professional. While it can be scary to think about, there’s some good news. If it’s caught early, some alcohol-related brain damage can be reversed by stopping or significantly reducing your drinking. Our brains have an amazing capacity for healing; research shows that after a period of abstinence, some cognitive functions can improve. A doctor can help you create a safe plan to cut back and can also check for common nutritional deficiencies, like a lack of thiamine (vitamin B1), which can contribute to brain-related issues.
For those who drink heavily and consistently, the stakes are higher. Repeated episodes of alcohol poisoning can lead to permanent brain damage and may result in severe conditions like Wernicke-Korsakoff syndrome. This is why professional medical advice is not just helpful—it's critical. If you have a physical dependence on alcohol, quitting abruptly without medical supervision can be dangerous and lead to severe withdrawal symptoms. A doctor can provide the support and resources needed to manage withdrawal safely, setting you on a path toward recovery without risking your health further. Please don't try to go it alone.
If you or a loved one is dealing with ARBD, recovery is centered on a few key strategies. The most critical action is to stop drinking alcohol, which halts further damage and gives the brain a chance to heal. Alongside this, nutrition plays a huge role. As mentioned, many heavy drinkers are deficient in thiamine, which can cause severe neurological problems like Wernicke's encephalopathy. A doctor will often recommend thiamine supplements and a balanced diet rich in vitamins and minerals. Engaging in cognitive exercises, staying physically active, and maintaining a structured daily routine can also support brain function and help rebuild neural pathways.
Protecting your brain doesn't have to be an all-or-nothing battle. It’s really about understanding your personal limits and creating habits that support responsible drinking. This shift in mindset is powerful because it puts you back in control. Instead of focusing on what you’re giving up, you can focus on what you’re gaining: better health, clearer thinking, and more energy. The key is to start small. You don’t have to overhaul your entire life overnight. Begin by simply becoming more aware of your patterns. How much are you really drinking in a week? How does it make you feel the next day?
Once you have a clearer picture, you can set realistic goals. Maybe it’s committing to two alcohol-free days a week or deciding you’ll have only one drink at your next social gathering. Tools and apps designed for habit change, like Reframe, can be incredibly helpful for tracking your progress and providing support when you need it. Exploring the world of non-alcoholic cocktails or finding new hobbies that don’t revolve around drinking can also make the process feel less like a sacrifice and more like an exciting new chapter. You can find answers to common questions about this process in our FAQ section.
A great way to build healthier habits is to practice mindful drinking. This just means being more present and intentional with your choices around alcohol. It’s about asking yourself *why* you want a drink instead of reaching for one automatically. A simple mindful technique is to always eat a meal before you drink. Having food in your stomach slows the absorption of alcohol, giving your body more time to process it. Other practices include sipping your drink slowly to savor it, alternating each alcoholic beverage with a glass of water, and pausing before you get a refill to check in with how you’re feeling.
What’s the difference between being really drunk and having alcohol poisoning? Think of it this way: being drunk affects your coordination, judgment, and mood. Alcohol poisoning is a medical emergency where the amount of alcohol in your bloodstream is so high that it starts to shut down the parts of your brain that control basic life-support functions. If you see someone who is confused, vomiting, breathing very slowly, or can't be woken up, it's no longer about being drunk—it's a potential overdose that requires an immediate 911 call.
Can just one night of heavy drinking cause permanent brain damage? A single episode of severe alcohol poisoning can cause permanent brain damage, but not in the way you might think. The immediate danger comes from the body being deprived of oxygen, either from breathing that slows or stops, or from seizures. This lack of oxygen can harm brain cells. The more gradual brain damage, often called ARBD, typically develops from a pattern of heavy drinking over many years.
If someone passes out from drinking, isn't it best to just let them sleep it off? This is one of the most dangerous myths about alcohol. A person's blood alcohol level can continue to rise even after they've stopped drinking and passed out. This means they can go from being unconscious to having a fatal overdose while they're "sleeping." They are also at serious risk of choking if they vomit, as their gag reflex is suppressed. An unconscious person needs monitoring and immediate medical help.
Is brain damage from alcohol always permanent? Not always. The brain has a remarkable ability to heal. When someone stops drinking, especially if the damage is caught early, they can often see improvements in their cognitive function and memory. The key is to stop the exposure to alcohol to prevent further harm and give the brain a chance to recover. However, in very severe and long-term cases, such as Wernicke-Korsakoff syndrome, the damage can be lasting.
How do I know if I’m binge drinking if I don’t feel that drunk? Binge drinking is defined by the amount of alcohol consumed in a short time, not by how you feel. It's typically defined as having four or more drinks for women, or five or more for men, within about two hours. It's easy to hit this number without realizing it, especially since many cocktails, glasses of wine, or craft beers contain more than one "standard" serving of alcohol. It’s about the math, not the buzz.

Research shows that excessive alcohol consumption can lead to liver cirrhosis — and even moderate drinking can cause liver damage over an extended period of time.
Ready to give your liver a break and change your drinking patterns? Although it isn’t a treatment for alcohol use disorder (AUD), the Reframe app can help you cut back or quit. Our science-backed program has helped millions of people around the world drink less and live more. And we want to help you get there, too!
When you download the Reframe app, you will get the knowledge and skills you need to not only survive drinking less, but to thrive throughout your journey. In addition to daily research-backed readings that teach you all about the neuroscience of alcohol, you will have access to our in-app Toolkit full of resources and activities to help you navigate any situation you find yourself in.
Meet millions of fellow Reframers just like you in our 24/7 Forum chat and daily Zoom check-in meetings to get encouragement and inspiration from people all over the world who are on a similar journey. We can also connect you with our licensed Reframe coaches for more personalized guidance.
With the Reframe app, you will never get bored: we’re constantly adding new features to improve your in-app experience. Meet our in-app chatbot, Melody, powered by the world’s most powerful AI technology — she is here to help as you adjust to a life with less (or no) alcohol.
And there’s more! Every month, we launch fun challenges — like Dry/Damp January, Mental Health May, and Outdoorsy June — for you to participate alongside fellow Reframers (or solo if you prefer!).
The Reframe app is free for 7 days, so you can download it today with absolutely no risk! Are you ready to feel empowered and discover life beyond alcohol? Can’t wait to welcome you into our caring and fun community!
There’s no way around it — cirrhosis, a severe liver disease primarily caused by excessive alcohol consumption, is a heavy topic. But before you start to panic, rest assured that a single glass of Chianti isn’t the culprit here. When it comes to risk, it’s all about the amount and frequency of alcohol consumption. So, how much alcohol causes cirrhosis? What are alcoholic cirrhosis symptoms? And what is liver cirrhosis treatment like? Let’s find out!
First, let’s talk about the causes and risk of liver cirrhosis. When we’re talking about booze, the reason it causes liver cirrhosis has to do with the way our body processes alcohol. First the liver transforms it into a toxic substance called acetaldehyde, and then into the non-toxic acetate. This two-step process is taxing for the liver, and it supersedes any other duties the liver might otherwise be fulfilling.
Our livers are incredibly resilient. They can take the hit of moderate alcohol consumption, heal, and regenerate. However, long-term heavy drinking can overwhelm this regeneration process, leading to scarring of the liver, called cirrhosis.
Cirrhosis is a late stage of scarring — also known as liver fibrosis — of the liver caused by the repeated process of damaged tissue repairing itself. Over time, as more and more scar tissue forms, the structure of the liver changes: it becomes hard and lumpy and starts to function less efficiently. Eventually, liver fibrosis can progress to cirrhosis.
This inefficient functioning of the liver can have a significant impact on our bodies. Our livers perform hundreds of vital functions: filtering toxins from our blood, aiding digestion, metabolizing drugs and hormones, storing vitamins and nutrients, and even helping clot our blood.
In the early stages of cirrhosis, one might not experience any symptoms. As cirrhosis progresses, symptoms and complications can develop that indicate the liver is severely damaged. These can include fatigue, easy bruising, jaundice (yellow discoloration of the skin and eyes), intense itching, fluid accumulation in the abdomen, loss of appetite, and confusion, drowsiness, and slurred speech.
Cirrhosis doesn't occur overnight. The liver damage that leads to cirrhosis is gradual, often taking many years of consistent heavy drinking. The initial stage, “alcoholic fatty liver disease,” is reversible. The next phase — alcoholic hepatitis — is when inflammation and liver cell damage start to occur. With the right steps, it’s still manageable; however, if heavy drinking continues, alcoholic cirrhosis becomes a real risk.
Unfortunately, once cirrhosis is present it tends to be permanent; it's very difficult to repair the damaged liver tissue. However, if the cirrhosis is diagnosed early enough, damage can be minimized by treating the underlying cause or various complications arising from it. As far as liver cirrhosis treatment goes, this usually means setting booze aside. In severe cases of cirrhosis, liver transplantation may be the only treatment option.

Now for the million-dollar question: how much alcohol causes cirrhosis? There is no neat, one-size-fits-all answer, unfortunately. The process is complex, and it depends on a variety of factors such as drinking patterns, body weight, age, and genetics.
As a general rule, though, men who consume more than 3-4 drinks per day and women who have 2-3 drinks daily over a period of 10 to 12 years are more likely to develop cirrhosis. This might seem manageable, but keep in mind that one standard “drink” equals 14 grams of pure alcohol. That's about 1.5 ounces of distilled spirits, 5 ounces of wine, or 12 ounces of regular beer.
A common misconception is that cirrhosis is a problem for the “heavy drinkers” only. While it's true that the risk increases as consumption increases, even moderate drinking can, over time, contribute to liver disease. This is especially true if it’s combined with other liver stressors, like obesity or viral hepatitis. It's not just the number of drinks that count: it’s our overall health context.
What about if we’ve already been diagnosed — is drinking with cirrhosis an absolute no? Well, let’s just say it’s not the best idea. For one thing, it can exacerbate liver inflammation and increase the risk of liver failure. Drinking alcohol with cirrhosis can also increase the risk of developing other health complications, such as bleeding disorders, kidney problems, and an increased risk of liver cancer.
And occasional drinking with cirrhosis? Again, it’s best to tread carefully. It’s important to give our liver time to rest and recover to avoid making things worse, so even occasional drinking with cirrhosis can be asking for trouble.
It's not all doom and gloom! Just as our behavior contributed to the damage, our behavior has the power to help our livers heal. Cirrhosis is largely preventable by reducing alcohol consumption or abstaining entirely.
Here are some steps we can take on a journey to heal our liver:
Cirrhosis poses a very real threat to our liver, and alcohol consumption is its primary cause. But there’s no need to blame ourselves or dwell on past choices. Let’s empower ourselves with knowledge and make conscious decisions moving forward.
Our livers are some of the hardest workers in our bodies, and it's never too late to show them some love. Let's treat them kindly, and they'll pay us back in kind with health, vitality, and the freedom to enjoy life's pleasures.
There’s no way around it — cirrhosis, a severe liver disease primarily caused by excessive alcohol consumption, is a heavy topic. But before you start to panic, rest assured that a single glass of Chianti isn’t the culprit here. When it comes to risk, it’s all about the amount and frequency of alcohol consumption. So, how much alcohol causes cirrhosis? What are alcoholic cirrhosis symptoms? And what is liver cirrhosis treatment like? Let’s find out!
First, let’s talk about the causes and risk of liver cirrhosis. When we’re talking about booze, the reason it causes liver cirrhosis has to do with the way our body processes alcohol. First the liver transforms it into a toxic substance called acetaldehyde, and then into the non-toxic acetate. This two-step process is taxing for the liver, and it supersedes any other duties the liver might otherwise be fulfilling.
Our livers are incredibly resilient. They can take the hit of moderate alcohol consumption, heal, and regenerate. However, long-term heavy drinking can overwhelm this regeneration process, leading to scarring of the liver, called cirrhosis.
Cirrhosis is a late stage of scarring — also known as liver fibrosis — of the liver caused by the repeated process of damaged tissue repairing itself. Over time, as more and more scar tissue forms, the structure of the liver changes: it becomes hard and lumpy and starts to function less efficiently. Eventually, liver fibrosis can progress to cirrhosis.
This inefficient functioning of the liver can have a significant impact on our bodies. Our livers perform hundreds of vital functions: filtering toxins from our blood, aiding digestion, metabolizing drugs and hormones, storing vitamins and nutrients, and even helping clot our blood.
In the early stages of cirrhosis, one might not experience any symptoms. As cirrhosis progresses, symptoms and complications can develop that indicate the liver is severely damaged. These can include fatigue, easy bruising, jaundice (yellow discoloration of the skin and eyes), intense itching, fluid accumulation in the abdomen, loss of appetite, and confusion, drowsiness, and slurred speech.
Cirrhosis doesn't occur overnight. The liver damage that leads to cirrhosis is gradual, often taking many years of consistent heavy drinking. The initial stage, “alcoholic fatty liver disease,” is reversible. The next phase — alcoholic hepatitis — is when inflammation and liver cell damage start to occur. With the right steps, it’s still manageable; however, if heavy drinking continues, alcoholic cirrhosis becomes a real risk.
Unfortunately, once cirrhosis is present it tends to be permanent; it's very difficult to repair the damaged liver tissue. However, if the cirrhosis is diagnosed early enough, damage can be minimized by treating the underlying cause or various complications arising from it. As far as liver cirrhosis treatment goes, this usually means setting booze aside. In severe cases of cirrhosis, liver transplantation may be the only treatment option.

Now for the million-dollar question: how much alcohol causes cirrhosis? There is no neat, one-size-fits-all answer, unfortunately. The process is complex, and it depends on a variety of factors such as drinking patterns, body weight, age, and genetics.
As a general rule, though, men who consume more than 3-4 drinks per day and women who have 2-3 drinks daily over a period of 10 to 12 years are more likely to develop cirrhosis. This might seem manageable, but keep in mind that one standard “drink” equals 14 grams of pure alcohol. That's about 1.5 ounces of distilled spirits, 5 ounces of wine, or 12 ounces of regular beer.
A common misconception is that cirrhosis is a problem for the “heavy drinkers” only. While it's true that the risk increases as consumption increases, even moderate drinking can, over time, contribute to liver disease. This is especially true if it’s combined with other liver stressors, like obesity or viral hepatitis. It's not just the number of drinks that count: it’s our overall health context.
What about if we’ve already been diagnosed — is drinking with cirrhosis an absolute no? Well, let’s just say it’s not the best idea. For one thing, it can exacerbate liver inflammation and increase the risk of liver failure. Drinking alcohol with cirrhosis can also increase the risk of developing other health complications, such as bleeding disorders, kidney problems, and an increased risk of liver cancer.
And occasional drinking with cirrhosis? Again, it’s best to tread carefully. It’s important to give our liver time to rest and recover to avoid making things worse, so even occasional drinking with cirrhosis can be asking for trouble.
It's not all doom and gloom! Just as our behavior contributed to the damage, our behavior has the power to help our livers heal. Cirrhosis is largely preventable by reducing alcohol consumption or abstaining entirely.
Here are some steps we can take on a journey to heal our liver:
Cirrhosis poses a very real threat to our liver, and alcohol consumption is its primary cause. But there’s no need to blame ourselves or dwell on past choices. Let’s empower ourselves with knowledge and make conscious decisions moving forward.
Our livers are some of the hardest workers in our bodies, and it's never too late to show them some love. Let's treat them kindly, and they'll pay us back in kind with health, vitality, and the freedom to enjoy life's pleasures.

Worried you might be trapped by your genes? Dive into an engaging exploration of the genetics influencing Alcohol Use Disorder (AUD)! Our genes may map a potential path — but our choices powerfully influence our journey. Read on for insightful, actionable steps towards a healthier, happier life.
Imagine walking through a dense forest on a treasure hunt, knowing that the path to success is littered with dangerous pitfalls. This adventure parallels the journey of navigating our genes, a complex map that outlines our susceptibilities and strengths.
One possible pitfall is Alcohol Use Disorder (AUD), a condition in which drinking becomes a compulsive, detrimental habit — a hidden trap in our genetic forest.
But is the path to AUD pre-determined by our genes, or can we take an alternate route? If you’ve ever turned to Google wondering whether you have the drinking problem that runs in your family, this might be the article for you.
Science has advanced significantly over the years, providing us with a deeper understanding of Alcohol Use Disorder (AUD) and its genetic underpinnings.
There is no single “alcoholic gene” that accounts for AUD. In fact, studies show that genetics account for about half the risk for AUD, meaning our genes influence our likelihood of developing AUD.
Among the 11 pairs of genes associated with an increased risk of developing AUD, here are some of the most common:

While genetic tests are available, it’s still a developing science — and it cannot guarantee the "catching" or preventing of AUD. Any concerns we have about our genetic risks should be discussed with our healthcare provider.
Family history and our childhood environment play a big role, too. This includes whether the following stressors were a part of our upbringing:
It's important to remember that our genetic makeup is not our destiny — it’s only part of the story. Even if our family history included major stressors, such as those listed above, it doesn’t guarantee we’ll develop AUD. Current stressors, life circumstances, and our everyday choices also play a role.
Our genes don’t dictate our journey. Genes play a part, but so do environmental factors — such as our upbringing, job, stressors, social influences, and coping strategies, to name a few.
Knowing the signs of AUD helps us avoid the hidden pitfalls. They range from less severe symptoms (like repeatedly drinking more than we intend) to severe symptoms (such as feeling unable to cut back on drinking, neglecting personal and professional responsibilities, and experiencing withdrawal symptoms when we’re not under the influence).
Much like spotting a trap in the forest, recognizing these signs is the first step towards choosing a safer path. By acknowledging these symptoms, we can start to navigate around the dangers and make decisions that lead us to healthier destinations.
Now that we understand our path isn't solely dictated by our genes and we can identify the signs of AUD, let's talk about how to steer clear of this pitfall.
Our genes may point us towards a risky path, but it's within our power to choose a safer route.
Alcohol Use Disorder, like a hidden trap, is a real and significant risk — but with knowledge, self-awareness, support, and actionable steps, we can navigate around it.
Remember, the goal isn't to fear the forest but to understand its dangers and equip ourselves with the right tools to navigate through it.
Embrace the journey, knowing that every step we take towards reducing our drinking is a step towards a healthier, happier life.

Although it isn’t a treatment for alcohol use disorder (AUD), the Reframe app can help you cut back on drinking gradually, with the science-backed knowledge to empower you 100% of the way. Our proven program has helped millions of people around the world drink less and live more. And we want to help you get there, too!
The Reframe app equips you with the knowledge and skills you need to not only survive drinking less, but to thrive while you navigate the journey. Our daily research-backed readings teach you the neuroscience of alcohol, and our in-app Toolkit provides the resources and activities you need to navigate each challenge.
You’ll meet millions of fellow Reframers in our 24/7 Forum chat and daily Zoom check-in meetings. Receive encouragement from people worldwide who know exactly what you’re going through! You’ll also have the opportunity to connect with our licensed Reframe coaches for more personalized guidance.
Plus, we’re always introducing new features to optimize your in-app experience. We recently launched our in-app chatbot, Melody, powered by the world’s most powerful AI technology. Melody is here to help as you adjust to a life with less (or no) alcohol.
And that’s not all! Every month, we launch fun challenges, like Dry/Damp January, Mental Health May, and Outdoorsy June. You won’t want to miss out on the chance to participate alongside fellow Reframers (or solo if that’s more your thing!).
The Reframe app is free for 7 days, so you don’t have anything to lose by trying it. Are you ready to feel empowered and discover life beyond alcohol? Then download our app today!
Imagine walking through a dense forest on a treasure hunt, knowing that the path to success is littered with dangerous pitfalls. This adventure parallels the journey of navigating our genes, a complex map that outlines our susceptibilities and strengths.
One possible pitfall is Alcohol Use Disorder (AUD), a condition in which drinking becomes a compulsive, detrimental habit — a hidden trap in our genetic forest.
But is the path to AUD pre-determined by our genes, or can we take an alternate route? If you’ve ever turned to Google wondering whether you have the drinking problem that runs in your family, this might be the article for you.
Science has advanced significantly over the years, providing us with a deeper understanding of Alcohol Use Disorder (AUD) and its genetic underpinnings.
There is no single “alcoholic gene” that accounts for AUD. In fact, studies show that genetics account for about half the risk for AUD, meaning our genes influence our likelihood of developing AUD.
Among the 11 pairs of genes associated with an increased risk of developing AUD, here are some of the most common:

While genetic tests are available, it’s still a developing science — and it cannot guarantee the "catching" or preventing of AUD. Any concerns we have about our genetic risks should be discussed with our healthcare provider.
Family history and our childhood environment play a big role, too. This includes whether the following stressors were a part of our upbringing:
It's important to remember that our genetic makeup is not our destiny — it’s only part of the story. Even if our family history included major stressors, such as those listed above, it doesn’t guarantee we’ll develop AUD. Current stressors, life circumstances, and our everyday choices also play a role.
Our genes don’t dictate our journey. Genes play a part, but so do environmental factors — such as our upbringing, job, stressors, social influences, and coping strategies, to name a few.
Knowing the signs of AUD helps us avoid the hidden pitfalls. They range from less severe symptoms (like repeatedly drinking more than we intend) to severe symptoms (such as feeling unable to cut back on drinking, neglecting personal and professional responsibilities, and experiencing withdrawal symptoms when we’re not under the influence).
Much like spotting a trap in the forest, recognizing these signs is the first step towards choosing a safer path. By acknowledging these symptoms, we can start to navigate around the dangers and make decisions that lead us to healthier destinations.
Now that we understand our path isn't solely dictated by our genes and we can identify the signs of AUD, let's talk about how to steer clear of this pitfall.
Our genes may point us towards a risky path, but it's within our power to choose a safer route.
Alcohol Use Disorder, like a hidden trap, is a real and significant risk — but with knowledge, self-awareness, support, and actionable steps, we can navigate around it.
Remember, the goal isn't to fear the forest but to understand its dangers and equip ourselves with the right tools to navigate through it.
Embrace the journey, knowing that every step we take towards reducing our drinking is a step towards a healthier, happier life.

Although it isn’t a treatment for alcohol use disorder (AUD), the Reframe app can help you cut back on drinking gradually, with the science-backed knowledge to empower you 100% of the way. Our proven program has helped millions of people around the world drink less and live more. And we want to help you get there, too!
The Reframe app equips you with the knowledge and skills you need to not only survive drinking less, but to thrive while you navigate the journey. Our daily research-backed readings teach you the neuroscience of alcohol, and our in-app Toolkit provides the resources and activities you need to navigate each challenge.
You’ll meet millions of fellow Reframers in our 24/7 Forum chat and daily Zoom check-in meetings. Receive encouragement from people worldwide who know exactly what you’re going through! You’ll also have the opportunity to connect with our licensed Reframe coaches for more personalized guidance.
Plus, we’re always introducing new features to optimize your in-app experience. We recently launched our in-app chatbot, Melody, powered by the world’s most powerful AI technology. Melody is here to help as you adjust to a life with less (or no) alcohol.
And that’s not all! Every month, we launch fun challenges, like Dry/Damp January, Mental Health May, and Outdoorsy June. You won’t want to miss out on the chance to participate alongside fellow Reframers (or solo if that’s more your thing!).
The Reframe app is free for 7 days, so you don’t have anything to lose by trying it. Are you ready to feel empowered and discover life beyond alcohol? Then download our app today!

Learn the most common alcohol intolerance symptoms, what causes them, and how to manage reactions for a safer, more comfortable drinking experience.
Although it isn’t a treatment for alcohol use disorder (AUD), the Reframe app can help you cut back on drinking gradually, with the science-backed knowledge to empower you 100% of the way. Our proven program has helped millions of people around the world drink less and live more. And we want to help you get there, too!
The Reframe app equips you with the knowledge and skills you need to not only survive drinking less, but to thrive while you navigate the journey. Our daily research-backed readings teach you the neuroscience of alcohol, and our in-app Toolkit provides the resources and activities you need to navigate each challenge.
You’ll meet millions of fellow Reframers in our 24/7 Forum chat and daily Zoom check-in meetings. Receive encouragement from people worldwide who know exactly what you’re going through! You’ll also have the opportunity to connect with our licensed Reframe coaches for more personalized guidance.
Plus, we’re always introducing new features to optimize your in-app experience. We recently launched our in-app chatbot, Melody, powered by the world’s most powerful AI technology. Melody is here to help as you adjust to a life with less (or no) alcohol.
And that’s not all! Every month, we launch fun challenges, like Dry/Damp January, Mental Health May, and Outdoorsy June. You won’t want to miss out on the chance to participate alongside fellow Reframers (or solo if that’s more your thing!).
The Reframe app is free for 7 days, so you don’t have anything to lose by trying it. Are you ready to feel empowered and discover life beyond alcohol? Then download our app today!
Alcohol can be the life of the party. But for some of us, it’s the guest that makes everyone uncomfortable. If a single drink leaves you with a flushed face, an upset stomach, or a racing heart, your body is telling you something isn't right. These reactions can turn a fun night out into a stressful one. You might even wonder, can you be allergic to alcohol? While a true alcohol allergy is rare, these are often classic alcohol intolerance symptoms. Understanding what’s happening is the key to feeling more in control.
This is what being allergic to alcohol feels like. What are some signs you're allergic to alcohol? And can you be sensitive to a particular type — for example, can you be allergic to tequila? Or can you be allergic to whiskey? In this article, we’ll explore the differences between the two — and how to know if either could be impacting you.

In an allergy to alcohol, the immune system mistakenly identifies it as a threat and mounts an aggressive response.
Our body perceives the presence of alcohol as a life-threatening situation, and it sends our immune system into overdrive.
Some of us may be wondering, does being allergic to alcohol the same as having alcohol intolerance? Not quite. Alcohol intolerance can cause a variety of physical symptoms, similar to how a person can start sneezing after a strong spray of perfume. Our bodies can respond to alcohol as an irritant, causing adverse reactions that are often misunderstood.
While our immune system is behind alcohol allergies, alcohol intolerance is caused by a glitch in alcohol metabolism. The liver is at the center of this process, converting alcohol to acetaldehyde — a compound that’s more toxic than alcohol itself, which then gets converted into harmless acetic acid. Occasionally genetic variations lead to an enzyme deficiency that throws a wrench in the process, leading to acetaldehyde buildup. The result? We experience unpleasant symptoms, such as flushing, nausea, and rapid heartbeat after drinking.

Let's clear up a common misunderstanding: the symptoms of alcohol intolerance are not the same as feeling tipsy or drunk. When you have this condition, your body reacts almost immediately after you start drinking. One of the most telling signs is the "alcohol flush syndrome," where your face, neck, and even your chest can become warm and noticeably red. This isn't the gradual buzz that comes with intoxication; it's a swift, physical response from your digestive system signaling that it's struggling to process the alcohol. It's a distinct reaction that happens because your body can't properly break down the toxins in what you're drinking.
This reaction happens because of a specific genetic trait. Your body has an enzyme called ALDH2 that's supposed to help break down alcohol. If you have alcohol intolerance, this enzyme doesn't work as it should, causing a rapid buildup of a toxic compound called acetaldehyde. This is very different from an allergic reaction, which involves your immune system, and it's also distinct from the psychoactive effects of getting drunk. It’s a metabolic issue, plain and simple, and it’s why even a small amount of alcohol can trigger such an uncomfortable response.
Alcohol allergies are extremely rare, but when they occur, they can lead to severe symptoms:
An allergy to alcohol can be life-threatening. If you suspect you have an allergic reaction to alcohol, steer clear of it entirely until you’ve consulted with your healthcare provider.
As for the question of whether you can be allergic to a specific type of alcohol, the answer is yes. It all depends on the exact ingredient that’s causing the allergy — it might not be alcohol at all. For example, some people are allergic to grapes and can’t drink wine, but don’t have the same allergic reaction to alcohol when it comes to other types. And can you be allergic to whiskey or tequila? It’s rare but possible. In the case of whiskey, you might be allergic to specific grains that are used in the fermentation process, while in the case of tequila the culprit might be agave.
There is no cure for an alcohol allergy, so the best way to manage it is to avoid alcohol entirely. Treatment focuses on managing symptoms with antihistamines if accidental exposure occurs — however, doing so on a regular basis isn’t a good idea. And remember — always reach out for medical help if you have any concerns.
Unlike a true allergy, alcohol intolerance is a metabolic disorder, meaning your body can't process alcohol properly. The symptoms are uncomfortable and are your body’s way of telling you something isn’t right. These reactions usually happen soon after you have a drink. Recognizing them is the first step toward understanding your body’s relationship with alcohol and making choices that support your well-being.
One of the most common and visible signs of alcohol intolerance is facial flushing. You might notice your face, neck, or chest turning red and feeling warm shortly after drinking. This happens because blood vessels in your skin dilate in response to the buildup of acetaldehyde, a toxic compound your body creates when it metabolizes alcohol. According to the Mayo Clinic, this distinct blushing is a key symptom of the condition. While it might seem like a minor inconvenience, it's a clear signal that your system is struggling to break down alcohol efficiently.
Feeling dizzy, lightheaded, or even nauseous after just a small amount of alcohol could also point to an intolerance. These symptoms can be linked to a drop in blood pressure. When your body can't process alcohol correctly, it can trigger a reaction that affects your cardiovascular system. The Cleveland Clinic notes that low blood pressure, along with feeling sick to your stomach or vomiting, is a common reaction. It’s easy to mistake this for simply having a low tolerance for alcohol, but it’s actually a specific physiological response to a substance your body can’t handle.
If you have asthma, you might notice your symptoms flare up after drinking alcohol. This isn't a coincidence. For some people, alcohol intolerance can aggravate pre-existing respiratory conditions. The ingredients in alcoholic beverages, such as sulfites or histamine, can act as triggers for asthma attacks. The Mayo Clinic includes worsening asthma as a potential symptom of alcohol intolerance. If you find yourself reaching for your inhaler after a glass of wine or beer, it could be a sign that your body is reacting negatively to something in your drink.
So, what’s happening inside your body to cause these reactions? Alcohol intolerance isn't about willpower or how much you're used to drinking. It's a biological process that you can't control. The primary cause is genetic, specifically related to an enzyme that's supposed to help you digest alcohol. However, sometimes the issue isn't with the alcohol (ethanol) itself but with other ingredients commonly found in alcoholic drinks.
The main culprit behind alcohol intolerance is often a faulty enzyme called aldehyde dehydrogenase 2 (ALDH2). When you drink, your liver first breaks down alcohol into a toxic compound called acetaldehyde. Then, the ALDH2 enzyme is supposed to swoop in and break that down into a harmless substance. But if you have an ALDH2 deficiency, this enzyme doesn't work correctly. As a result, acetaldehyde builds up in your blood, causing those unpleasant symptoms like flushing and nausea. It’s a genetic hiccup in your body’s natural detoxification process.
This ALDH2 deficiency is a genetic trait passed down through families. It's most commonly found in people of East Asian descent, which is why facial flushing after drinking is sometimes referred to as "Asian flush" or "Asian glow." However, it's important to remember that anyone can have this genetic variation. According to the Mayo Clinic, while it's most often seen in people of Asian background, this genetic trait can appear in any ethnicity. If your parents have alcohol intolerance, there's a higher chance you might have it, too.
Sometimes, you might experience a reaction that seems like alcohol intolerance, but the alcohol itself isn't the problem. Alcoholic beverages are complex mixtures containing various ingredients that can trigger symptoms. Things like sulfites, histamine, or even specific grains like wheat or barley could be the real cause of your discomfort. This is why you might react to one type of drink, like red wine, but feel fine after another, like vodka. Pinpointing the exact trigger can help you make more informed choices about what you drink.
Sulfites are preservatives that are commonly added to beer and wine to prevent spoilage and oxidation. While they are generally safe for most people, some individuals are sensitive to them. For these people, consuming sulfites can lead to allergy-like symptoms, including breathing problems (especially in those with asthma), hives, and digestive upset. If you find that you primarily react to wine, sulfites could be the reason.
Histamine is another compound that can cause issues. It's produced during the fermentation process by yeast and bacteria and is found in high amounts in certain alcoholic drinks, particularly aged red wines. Your body naturally produces enzymes to break down histamine, but some people don't produce enough. When histamine builds up, it can cause symptoms like headaches, nasal congestion, skin flushing, and digestive problems, which can easily be mistaken for alcohol intolerance.
Ignoring the signs of alcohol intolerance and continuing to drink can do more than just cause temporary discomfort. It can lead to serious health problems down the road. When your body can't break down acetaldehyde effectively, this toxic compound circulates in your system, causing damage to your cells over time. Listening to your body's warning signals is a key part of mindful drinking and protecting your long-term health.
One of the most significant risks associated with drinking alcohol despite having an ALDH2 deficiency is an increased risk of certain cancers. The buildup of acetaldehyde is known to damage DNA and stop cells from repairing this damage, which can lead to cancerous growth. According to Cedars-Sinai, regularly drinking with this condition is linked to a much higher risk of developing cancers of the esophagus, mouth, and throat. It essentially exposes your body to a known carcinogen every time you drink.
Your liver bears the brunt of processing alcohol, and when it's constantly struggling with a buildup of acetaldehyde, it can lead to significant damage. The Cleveland Clinic warns that people with alcohol intolerance who drink regularly have a higher risk for liver diseases, including cirrhosis, which is severe scarring of the liver. Over time, this strain can also contribute to other health issues, including problems with your heart and digestive system, making it crucial to take symptoms of intolerance seriously.
Armed with this knowledge, we can take steps to handle our unexpected guest or, better yet, not invite them at all. Here are seven actionable steps to reevaluate our relationship with alcohol:
Understanding alcohol intolerance and allergy allows us to consider our relationship with alcohol and take strides towards healthier choices. If you think you have an allergy, speak to your healthcare provider. Most likely, they’ll tell you to cut alcohol out entirely and in any form.
If you suspect you have an alcohol intolerance, your body is sending you clear signals. The next step is to listen and respond thoughtfully. Managing intolerance isn't about finding ways to push through the discomfort; it's about understanding what your body needs and adjusting your habits to support your long-term health. This process starts with getting a clear picture of what’s happening, which means turning to a professional for guidance instead of trying to figure it all out on your own. From there, you can build a strategy that feels right for you.
The first and most important step is to talk to your doctor. They can help you confirm whether you have an intolerance and rule out other potential causes for your symptoms. Your doctor will likely start by asking detailed questions about what happens when you drink alcohol — what you drink, how much, and the specific reactions you experience. To get a more definitive answer, they might perform a simple diagnostic procedure to observe how your skin reacts directly to alcohol.
One common method your doctor might use is the ethanol patch test. It’s a straightforward and quick procedure where a drop of ethanol (pure alcohol) is placed on a gauze pad and taped to your arm. After about seven minutes, the doctor will remove the patch and check the area for a reaction. If your skin becomes red, itchy, or swollen, it’s a strong indicator that you have an alcohol intolerance. This simple test can provide the clarity you need to move forward with a management plan.
It can be tempting to pop an antihistamine or an antacid before a night out to prevent the uncomfortable symptoms of alcohol intolerance. However, this is a risky strategy. Masking your symptoms doesn't address the root issue; it only tricks you into thinking you can handle more alcohol than your body is equipped to process. This can lead you to drink more, putting you at risk for more severe health problems down the line. Your body’s reaction is a warning sign, and covering it up doesn’t make the danger go away.
The most effective way to manage alcohol intolerance is also the simplest: avoid or significantly limit your alcohol intake. When your body reacts with flushing, nausea, or a headache, it’s telling you that alcohol isn't safe for it. Trying to "gut through" the discomfort ignores these crucial signals. Instead, this is an opportunity to practice mindful drinking. Pay close attention to how you feel, honor your body’s limits, and explore the vibrant world of alcohol-free alternatives that won’t leave you feeling unwell.
If you suddenly start experiencing symptoms after drinking, it’s time to schedule a visit with your doctor to figure out the cause. It’s also important to be honest with yourself and your doctor about your drinking patterns. If you find that you continue to drink heavily despite feeling sick every time, it could be a sign of something more serious. A healthcare professional can provide compassionate support and resources to help you change your relationship with alcohol for good.
What's the real difference between an alcohol allergy and an intolerance? Think of it this way: an allergy is your immune system overreacting, treating alcohol like a dangerous invader. This can cause severe reactions like hives, swelling, and difficulty breathing. An intolerance, on the other hand, is a digestive issue. Your body lacks the right enzyme to break down alcohol properly, which leads to uncomfortable symptoms like facial flushing and nausea. While both are unpleasant, an allergy is an immune response, while an intolerance is a metabolic one.
I get a red, flushed face when I drink. Is that a big deal? That red face, often called "alcohol flush," is more than just a cosmetic issue. It's a clear sign that your body is struggling to process alcohol, causing a toxic compound called acetaldehyde to build up in your system. While it might seem harmless, consistently drinking when you have this reaction is linked to serious long-term health risks, including a higher chance of developing certain cancers. It's your body's way of sending a very direct warning signal.
Why do I only react to certain drinks, like red wine, but not others? This is a great question, and it often comes down to the other ingredients in your drink. It might not be the alcohol (ethanol) that's causing your symptoms. Red wine, for example, is high in compounds like sulfites and histamine, which are common triggers for allergy-like reactions in sensitive people. You might be reacting to one of these components rather than the alcohol itself, which explains why you can drink something purer, like vodka, without the same issue.
Is it safe to just take an antihistamine before drinking to stop the reaction? This is a risky approach that I wouldn't recommend. Taking an antihistamine might cover up the outward symptoms like flushing or a stuffy nose, but it does nothing to stop the internal process. Your body is still struggling to break down the alcohol and acetaldehyde is still building up. Masking the symptoms can give you a false sense of security, potentially leading you to drink more than your body can handle and increasing your risk of long-term damage.
I never used to have a problem with alcohol. Can you develop an intolerance later in life? Yes, it's possible to notice symptoms of intolerance suddenly, even if you've been drinking for years without any issues. Sometimes this can be linked to other factors, like developing new health conditions or starting certain medications. If you suddenly start reacting poorly to alcohol, it's a good idea to talk to your doctor. They can help you figure out the underlying cause and give you the best advice for moving forward.
Alcohol can be the life of the party. But for some of us, it’s the guest that makes everyone uncomfortable. If a single drink leaves you with a flushed face, an upset stomach, or a racing heart, your body is telling you something isn't right. These reactions can turn a fun night out into a stressful one. You might even wonder, can you be allergic to alcohol? While a true alcohol allergy is rare, these are often classic alcohol intolerance symptoms. Understanding what’s happening is the key to feeling more in control.
This is what being allergic to alcohol feels like. What are some signs you're allergic to alcohol? And can you be sensitive to a particular type — for example, can you be allergic to tequila? Or can you be allergic to whiskey? In this article, we’ll explore the differences between the two — and how to know if either could be impacting you.

In an allergy to alcohol, the immune system mistakenly identifies it as a threat and mounts an aggressive response.
Our body perceives the presence of alcohol as a life-threatening situation, and it sends our immune system into overdrive.
Some of us may be wondering, does being allergic to alcohol the same as having alcohol intolerance? Not quite. Alcohol intolerance can cause a variety of physical symptoms, similar to how a person can start sneezing after a strong spray of perfume. Our bodies can respond to alcohol as an irritant, causing adverse reactions that are often misunderstood.
While our immune system is behind alcohol allergies, alcohol intolerance is caused by a glitch in alcohol metabolism. The liver is at the center of this process, converting alcohol to acetaldehyde — a compound that’s more toxic than alcohol itself, which then gets converted into harmless acetic acid. Occasionally genetic variations lead to an enzyme deficiency that throws a wrench in the process, leading to acetaldehyde buildup. The result? We experience unpleasant symptoms, such as flushing, nausea, and rapid heartbeat after drinking.

Let's clear up a common misunderstanding: the symptoms of alcohol intolerance are not the same as feeling tipsy or drunk. When you have this condition, your body reacts almost immediately after you start drinking. One of the most telling signs is the "alcohol flush syndrome," where your face, neck, and even your chest can become warm and noticeably red. This isn't the gradual buzz that comes with intoxication; it's a swift, physical response from your digestive system signaling that it's struggling to process the alcohol. It's a distinct reaction that happens because your body can't properly break down the toxins in what you're drinking.
This reaction happens because of a specific genetic trait. Your body has an enzyme called ALDH2 that's supposed to help break down alcohol. If you have alcohol intolerance, this enzyme doesn't work as it should, causing a rapid buildup of a toxic compound called acetaldehyde. This is very different from an allergic reaction, which involves your immune system, and it's also distinct from the psychoactive effects of getting drunk. It’s a metabolic issue, plain and simple, and it’s why even a small amount of alcohol can trigger such an uncomfortable response.
Alcohol allergies are extremely rare, but when they occur, they can lead to severe symptoms:
An allergy to alcohol can be life-threatening. If you suspect you have an allergic reaction to alcohol, steer clear of it entirely until you’ve consulted with your healthcare provider.
As for the question of whether you can be allergic to a specific type of alcohol, the answer is yes. It all depends on the exact ingredient that’s causing the allergy — it might not be alcohol at all. For example, some people are allergic to grapes and can’t drink wine, but don’t have the same allergic reaction to alcohol when it comes to other types. And can you be allergic to whiskey or tequila? It’s rare but possible. In the case of whiskey, you might be allergic to specific grains that are used in the fermentation process, while in the case of tequila the culprit might be agave.
There is no cure for an alcohol allergy, so the best way to manage it is to avoid alcohol entirely. Treatment focuses on managing symptoms with antihistamines if accidental exposure occurs — however, doing so on a regular basis isn’t a good idea. And remember — always reach out for medical help if you have any concerns.
Unlike a true allergy, alcohol intolerance is a metabolic disorder, meaning your body can't process alcohol properly. The symptoms are uncomfortable and are your body’s way of telling you something isn’t right. These reactions usually happen soon after you have a drink. Recognizing them is the first step toward understanding your body’s relationship with alcohol and making choices that support your well-being.
One of the most common and visible signs of alcohol intolerance is facial flushing. You might notice your face, neck, or chest turning red and feeling warm shortly after drinking. This happens because blood vessels in your skin dilate in response to the buildup of acetaldehyde, a toxic compound your body creates when it metabolizes alcohol. According to the Mayo Clinic, this distinct blushing is a key symptom of the condition. While it might seem like a minor inconvenience, it's a clear signal that your system is struggling to break down alcohol efficiently.
Feeling dizzy, lightheaded, or even nauseous after just a small amount of alcohol could also point to an intolerance. These symptoms can be linked to a drop in blood pressure. When your body can't process alcohol correctly, it can trigger a reaction that affects your cardiovascular system. The Cleveland Clinic notes that low blood pressure, along with feeling sick to your stomach or vomiting, is a common reaction. It’s easy to mistake this for simply having a low tolerance for alcohol, but it’s actually a specific physiological response to a substance your body can’t handle.
If you have asthma, you might notice your symptoms flare up after drinking alcohol. This isn't a coincidence. For some people, alcohol intolerance can aggravate pre-existing respiratory conditions. The ingredients in alcoholic beverages, such as sulfites or histamine, can act as triggers for asthma attacks. The Mayo Clinic includes worsening asthma as a potential symptom of alcohol intolerance. If you find yourself reaching for your inhaler after a glass of wine or beer, it could be a sign that your body is reacting negatively to something in your drink.
So, what’s happening inside your body to cause these reactions? Alcohol intolerance isn't about willpower or how much you're used to drinking. It's a biological process that you can't control. The primary cause is genetic, specifically related to an enzyme that's supposed to help you digest alcohol. However, sometimes the issue isn't with the alcohol (ethanol) itself but with other ingredients commonly found in alcoholic drinks.
The main culprit behind alcohol intolerance is often a faulty enzyme called aldehyde dehydrogenase 2 (ALDH2). When you drink, your liver first breaks down alcohol into a toxic compound called acetaldehyde. Then, the ALDH2 enzyme is supposed to swoop in and break that down into a harmless substance. But if you have an ALDH2 deficiency, this enzyme doesn't work correctly. As a result, acetaldehyde builds up in your blood, causing those unpleasant symptoms like flushing and nausea. It’s a genetic hiccup in your body’s natural detoxification process.
This ALDH2 deficiency is a genetic trait passed down through families. It's most commonly found in people of East Asian descent, which is why facial flushing after drinking is sometimes referred to as "Asian flush" or "Asian glow." However, it's important to remember that anyone can have this genetic variation. According to the Mayo Clinic, while it's most often seen in people of Asian background, this genetic trait can appear in any ethnicity. If your parents have alcohol intolerance, there's a higher chance you might have it, too.
Sometimes, you might experience a reaction that seems like alcohol intolerance, but the alcohol itself isn't the problem. Alcoholic beverages are complex mixtures containing various ingredients that can trigger symptoms. Things like sulfites, histamine, or even specific grains like wheat or barley could be the real cause of your discomfort. This is why you might react to one type of drink, like red wine, but feel fine after another, like vodka. Pinpointing the exact trigger can help you make more informed choices about what you drink.
Sulfites are preservatives that are commonly added to beer and wine to prevent spoilage and oxidation. While they are generally safe for most people, some individuals are sensitive to them. For these people, consuming sulfites can lead to allergy-like symptoms, including breathing problems (especially in those with asthma), hives, and digestive upset. If you find that you primarily react to wine, sulfites could be the reason.
Histamine is another compound that can cause issues. It's produced during the fermentation process by yeast and bacteria and is found in high amounts in certain alcoholic drinks, particularly aged red wines. Your body naturally produces enzymes to break down histamine, but some people don't produce enough. When histamine builds up, it can cause symptoms like headaches, nasal congestion, skin flushing, and digestive problems, which can easily be mistaken for alcohol intolerance.
Ignoring the signs of alcohol intolerance and continuing to drink can do more than just cause temporary discomfort. It can lead to serious health problems down the road. When your body can't break down acetaldehyde effectively, this toxic compound circulates in your system, causing damage to your cells over time. Listening to your body's warning signals is a key part of mindful drinking and protecting your long-term health.
One of the most significant risks associated with drinking alcohol despite having an ALDH2 deficiency is an increased risk of certain cancers. The buildup of acetaldehyde is known to damage DNA and stop cells from repairing this damage, which can lead to cancerous growth. According to Cedars-Sinai, regularly drinking with this condition is linked to a much higher risk of developing cancers of the esophagus, mouth, and throat. It essentially exposes your body to a known carcinogen every time you drink.
Your liver bears the brunt of processing alcohol, and when it's constantly struggling with a buildup of acetaldehyde, it can lead to significant damage. The Cleveland Clinic warns that people with alcohol intolerance who drink regularly have a higher risk for liver diseases, including cirrhosis, which is severe scarring of the liver. Over time, this strain can also contribute to other health issues, including problems with your heart and digestive system, making it crucial to take symptoms of intolerance seriously.
Armed with this knowledge, we can take steps to handle our unexpected guest or, better yet, not invite them at all. Here are seven actionable steps to reevaluate our relationship with alcohol:
Understanding alcohol intolerance and allergy allows us to consider our relationship with alcohol and take strides towards healthier choices. If you think you have an allergy, speak to your healthcare provider. Most likely, they’ll tell you to cut alcohol out entirely and in any form.
If you suspect you have an alcohol intolerance, your body is sending you clear signals. The next step is to listen and respond thoughtfully. Managing intolerance isn't about finding ways to push through the discomfort; it's about understanding what your body needs and adjusting your habits to support your long-term health. This process starts with getting a clear picture of what’s happening, which means turning to a professional for guidance instead of trying to figure it all out on your own. From there, you can build a strategy that feels right for you.
The first and most important step is to talk to your doctor. They can help you confirm whether you have an intolerance and rule out other potential causes for your symptoms. Your doctor will likely start by asking detailed questions about what happens when you drink alcohol — what you drink, how much, and the specific reactions you experience. To get a more definitive answer, they might perform a simple diagnostic procedure to observe how your skin reacts directly to alcohol.
One common method your doctor might use is the ethanol patch test. It’s a straightforward and quick procedure where a drop of ethanol (pure alcohol) is placed on a gauze pad and taped to your arm. After about seven minutes, the doctor will remove the patch and check the area for a reaction. If your skin becomes red, itchy, or swollen, it’s a strong indicator that you have an alcohol intolerance. This simple test can provide the clarity you need to move forward with a management plan.
It can be tempting to pop an antihistamine or an antacid before a night out to prevent the uncomfortable symptoms of alcohol intolerance. However, this is a risky strategy. Masking your symptoms doesn't address the root issue; it only tricks you into thinking you can handle more alcohol than your body is equipped to process. This can lead you to drink more, putting you at risk for more severe health problems down the line. Your body’s reaction is a warning sign, and covering it up doesn’t make the danger go away.
The most effective way to manage alcohol intolerance is also the simplest: avoid or significantly limit your alcohol intake. When your body reacts with flushing, nausea, or a headache, it’s telling you that alcohol isn't safe for it. Trying to "gut through" the discomfort ignores these crucial signals. Instead, this is an opportunity to practice mindful drinking. Pay close attention to how you feel, honor your body’s limits, and explore the vibrant world of alcohol-free alternatives that won’t leave you feeling unwell.
If you suddenly start experiencing symptoms after drinking, it’s time to schedule a visit with your doctor to figure out the cause. It’s also important to be honest with yourself and your doctor about your drinking patterns. If you find that you continue to drink heavily despite feeling sick every time, it could be a sign of something more serious. A healthcare professional can provide compassionate support and resources to help you change your relationship with alcohol for good.
What's the real difference between an alcohol allergy and an intolerance? Think of it this way: an allergy is your immune system overreacting, treating alcohol like a dangerous invader. This can cause severe reactions like hives, swelling, and difficulty breathing. An intolerance, on the other hand, is a digestive issue. Your body lacks the right enzyme to break down alcohol properly, which leads to uncomfortable symptoms like facial flushing and nausea. While both are unpleasant, an allergy is an immune response, while an intolerance is a metabolic one.
I get a red, flushed face when I drink. Is that a big deal? That red face, often called "alcohol flush," is more than just a cosmetic issue. It's a clear sign that your body is struggling to process alcohol, causing a toxic compound called acetaldehyde to build up in your system. While it might seem harmless, consistently drinking when you have this reaction is linked to serious long-term health risks, including a higher chance of developing certain cancers. It's your body's way of sending a very direct warning signal.
Why do I only react to certain drinks, like red wine, but not others? This is a great question, and it often comes down to the other ingredients in your drink. It might not be the alcohol (ethanol) that's causing your symptoms. Red wine, for example, is high in compounds like sulfites and histamine, which are common triggers for allergy-like reactions in sensitive people. You might be reacting to one of these components rather than the alcohol itself, which explains why you can drink something purer, like vodka, without the same issue.
Is it safe to just take an antihistamine before drinking to stop the reaction? This is a risky approach that I wouldn't recommend. Taking an antihistamine might cover up the outward symptoms like flushing or a stuffy nose, but it does nothing to stop the internal process. Your body is still struggling to break down the alcohol and acetaldehyde is still building up. Masking the symptoms can give you a false sense of security, potentially leading you to drink more than your body can handle and increasing your risk of long-term damage.
I never used to have a problem with alcohol. Can you develop an intolerance later in life? Yes, it's possible to notice symptoms of intolerance suddenly, even if you've been drinking for years without any issues. Sometimes this can be linked to other factors, like developing new health conditions or starting certain medications. If you suddenly start reacting poorly to alcohol, it's a good idea to talk to your doctor. They can help you figure out the underlying cause and give you the best advice for moving forward.

Have your kidneys ever hurt after a night of heavy drinking? This isn’t uncommon. Explore how alcohol affects our kidneys and what we can do to keep them functioning optimally.
Although it isn’t a treatment for alcohol use disorder (AUD), the Reframe app can help you cut back on drinking gradually, with the science-backed knowledge to empower you 100% of the way. Our proven program has helped millions of people around the world drink less and live more. And we want to help you get there, too!
The Reframe app equips you with the knowledge and skills you need to not only survive drinking less, but to thrive while you navigate the journey. Our daily research-backed readings teach you the neuroscience of alcohol, and our in-app Toolkit provides the resources and activities you need to navigate each challenge.
You’ll meet millions of fellow Reframers in our 24/7 Forum chat and daily Zoom check-in meetings. Receive encouragement from people worldwide who know exactly what you’re going through! You’ll also have the opportunity to connect with our licensed Reframe coaches for more personalized guidance.
Plus, we’re always introducing new features to optimize your in-app experience. We recently launched our in-app chatbot, Melody, powered by the world’s most powerful AI technology. Melody is here to help as you adjust to a life with less (or no) alcohol.
And that’s not all! Every month, we launch fun challenges, like Dry/Damp January, Mental Health May, and Outdoorsy June. You won’t want to miss out on the chance to participate alongside fellow Reframers (or solo if that’s more your thing!).
The Reframe app is free for 7 days, so you don’t have anything to lose by trying it. Are you ready to feel empowered and discover life beyond alcohol? Then download our app through the App Store or Google Play today!
It always seems to happen: you meet some friends for a happy hour and end up having one drink too many. You go to bed way more tipsy than you would have liked, and when you wake up, you feel like you’ve been hit by a truck. But it’s not just the headache, nausea, and brain fog — it’s a weird pain deep in your abdomen. Is it possible that your kidneys are actually in pain from drinking alcohol?
Does alcohol affect kidneys? What does kidney pain after drinking mean? And can alcohol cause kidney stones? In this post, we’ll explore why our kidneys are so important and how alcohol affects their functioning. We’ll also offer tips for enhancing our kidney health. Let’s get started!

Before we dive into how alcohol affects our kidneys, it’s helpful to look at how our kidneys work and why they’re so important. We don’t often think about them, but these two small organs are as vital to our health as our heart and lungs, performing complex and vital functions that keep the rest of our body in balance.
Shaped like kidney beans (hence the name!), our kidneys are located deep in our abdomen, on either side of our spine. Consider them a filtration system: their main job is to remove waste products and excess fluid from our body.
Here’s how it works: every minute, about one liter of blood — or one-fifth of all the blood pumped by the heart — enters the kidneys through our arteries. This blood is cleaned by passing through millions of tiny blood filters, called nephrons. Any waste materials or excess fluid is passed into the bladder where it is stored as urine, while the newly-filtered blood returns to our bloodstream through our veins.
This process helps keep us alive: without a filtration system, we would poison ourselves with a buildup of toxins and waste. Our kidneys work hard day in and day out to prevent this from happening. In fact, every 24 hours, our kidneys filter and return to the bloodstream about 200 quarts of fluid. Approximately two quarts are eliminated from the body in the form of urine, while the remainder is retained in the body.
In addition to filtering the blood, our kidneys have 3 other important functions:
Interestingly, while most people are born with two kidneys, a person can live a normal and long life with only one healthy kidney. If one kidney is lost, the other kidney can increase its working capacity and provide up to 75% of normal kidney function. This is why people can donate a kidney to someone who needs it.

Now that we know how important and hard working our kidneys are, we can ask the next important question: does alcohol affect kidneys? Simply put: yes! This might not be all that surprising, given that alcohol is a toxin. After all, it’s their job to filter out toxic substances. But let’s take a closer look at 4 specific ways alcohol affects our kidneys:
One significant way alcohol affects our kidneys is by making it more difficult for them to function effectively. For instance, alcohol impairs the structure and function of the nephrons — those functional units of our kidneys responsible for filtering waste products and excess fluids. This can lead to a condition called acute kidney injury, which occurs when the toxins from alcohol build up in our body quickly and our kidneys can’t maintain the right fluid balance. Binge drinking in particular places a great strain on the kidneys and can cause acute kidney damage.
Furthermore, alcohol can affect kidney function by causing or exacerbating other health conditions that harm the kidneys. For example, alcohol is a known risk factor for high blood pressure, a leading cause of kidney damage. Additionally, excessive alcohol consumption can contribute to liver damage and disease, which can, in turn, impair kidney function. Furthermore, alcohol can interfere with the body's ability to regulate fluids and electrolytes, leading to dehydration and electrolyte imbalances that can strain the kidneys.
Finally let’s dispel a myth. Because alcohol is a diuretic, some might think it helps “flush out” the kidneys, but that’s not the case. In fact, it makes them work overtime while depleting the body of important nutrients and damaging the kidneys in the process.
So is beer — an especially potent diuretic — good for your kidneys? The answer is no. Just like other types of alcohol, beer can put unnecessary strain on the kidneys.
It could mean a kidney infection. Alcohol can also increase the risk of kidney infections, which typically start in the bladder and travel up the ureters to the kidneys. Alcohol impairs the immune system, making it more difficult for our body to fight off infections. Additionally, because alcohol can cause dehydration, this can lead to a higher concentration of bacteria in the urinary tract, increasing the risk of a urinary tract infection (UTI). UTIs that spread to the bladder may cause kidney pain and lead to a kidney infection.
Excessive alcohol consumption has been linked to an increased risk of developing chronic kidney disease (CKD), a long-term condition characterized by a gradual loss of kidney function. The likelihood is greater for individuals who already have other risk factors for the disease, such as high blood pressure or diabetes. Smokers who are heavy drinkers have about five times more chance of developing CKD than people who don’t smoke or drink alcohol to excess.
What are the first signs? While the symptoms below can be signs of many different conditions, they are some of the typical ones for CKD:
Alcohol can also interfere with the effectiveness of medications used to manage kidney disease and its complications. For example, alcohol can reduce the effectiveness of blood pressure medications, making it more difficult to control high blood pressure, a leading cause of CKD.
While alcohol consumption isn’t directly linked to kidney stones (hardened deposits formed from minerals and salts in the kidneys), research suggests it can contribute to their development and progression. They can be incredibly painful and sometimes require surgical intervention.
Since alcohol is dehydrating, it increases the concentration of minerals in our urine, which elevates the risk of stone formation. This risk is especially high during instances of binge drinking, which quickly depletes the body's water content. This is also why we might experience kidney pain after a night of heavy drinking.
Alcohol can also affect the balance of acid and alkaline substances in the urine. High levels of uric acid can lead to the formation of uric acid stones. Regular and heavy consumption of alcohol, especially beer and spirits, is associated with higher uric acid levels in the body.
Furthermore, alcohol can exacerbate the symptoms of kidney stones. It can increase the heart rate, leading to faster blood flow and potentially pushing the stones into the ureters, causing severe pain and possible obstruction.
It’s important to be aware of all the ways alcohol can affect our kidneys, as we might develop certain symptoms over time that indicate kidney damage — particularly if we’re consuming alcohol heavily over a long period of time. Plus, issues affecting the kidneys can quickly affect the rest of our body, potentially causing problems in multiple organs.
Watch for these signs that indicate we might have alcohol-related kidney damage:
Kidney pain may be felt in the upper or lower back or between the buttocks and lower ribs. The pain may be felt immediately after consuming alcohol or after we’ve stopped drinking. If we’re experiencing any of the above symptoms or suspect we might have kidney damage from alcohol use, it’s important to contact a medical health professional.
So, how is kidney damage treated — is there a cure? Well, that depends. Acute kidney damage caused by binge drinking will typically resolve itself within a few days. The damage can usually be reversed by stopping drinking and allowing our kidneys to recover. Keep in mind, however, that repeated episodes of binge drinking may cause irreversible damage.
As for chronic kidney disease, sadly there’s no cure. Treatment usually involves helping relieve symptoms and preventing it from getting worse. Our doctor might instruct us to manage our blood pressure levels, follow a kidney-friendly diet, and get adequate exercise.
Depending on the severity of our condition, doctors also might prescribe medications to manage symptoms. In extreme cases, CKD can lead to kidney failure, which may require a kidney transplant or dialysis — a mode of therapy in which a machine is used to perform the job of the kidneys. Untreated, complete kidney failure from alcohol will result in death.
The good news is that we have more control over the health of our kidneys than we might think. It’s worth making certain lifestyle changes, given how vital these organs are to our survival. In addition to limiting our alcohol consumption or eliminating it entirely, there are 5 ways we can keep our kidneys healthy and functioning optimally:
Our kidneys play a vital role in keeping us healthy and alive. They filter out toxins and waste and remove excess fluid from our body. Chronic, long-term alcohol consumption can damage our kidneys, leading to chronic kidney disease or failure. Even a single episode of binge drinking can put stress on our kidneys and cause acute kidney damage. Some of the best things we can do to keep our kidneys healthy include limiting our alcohol consumption, drinking plenty of water, eating a healthy diet, staying physically active, limiting our intake of over-the-counter pain relievers, and not smoking.
If you want to give your kidneys a boost by cutting back on your alcohol consumption, consider trying Reframe. We’re a neuroscience-backed app that has helped millions of people reduce their alcohol consumption and form healthier lifestyle habits.
It always seems to happen: you meet some friends for a happy hour and end up having one drink too many. You go to bed way more tipsy than you would have liked, and when you wake up, you feel like you’ve been hit by a truck. But it’s not just the headache, nausea, and brain fog — it’s a weird pain deep in your abdomen. Is it possible that your kidneys are actually in pain from drinking alcohol?
Does alcohol affect kidneys? What does kidney pain after drinking mean? And can alcohol cause kidney stones? In this post, we’ll explore why our kidneys are so important and how alcohol affects their functioning. We’ll also offer tips for enhancing our kidney health. Let’s get started!

Before we dive into how alcohol affects our kidneys, it’s helpful to look at how our kidneys work and why they’re so important. We don’t often think about them, but these two small organs are as vital to our health as our heart and lungs, performing complex and vital functions that keep the rest of our body in balance.
Shaped like kidney beans (hence the name!), our kidneys are located deep in our abdomen, on either side of our spine. Consider them a filtration system: their main job is to remove waste products and excess fluid from our body.
Here’s how it works: every minute, about one liter of blood — or one-fifth of all the blood pumped by the heart — enters the kidneys through our arteries. This blood is cleaned by passing through millions of tiny blood filters, called nephrons. Any waste materials or excess fluid is passed into the bladder where it is stored as urine, while the newly-filtered blood returns to our bloodstream through our veins.
This process helps keep us alive: without a filtration system, we would poison ourselves with a buildup of toxins and waste. Our kidneys work hard day in and day out to prevent this from happening. In fact, every 24 hours, our kidneys filter and return to the bloodstream about 200 quarts of fluid. Approximately two quarts are eliminated from the body in the form of urine, while the remainder is retained in the body.
In addition to filtering the blood, our kidneys have 3 other important functions:
Interestingly, while most people are born with two kidneys, a person can live a normal and long life with only one healthy kidney. If one kidney is lost, the other kidney can increase its working capacity and provide up to 75% of normal kidney function. This is why people can donate a kidney to someone who needs it.

Now that we know how important and hard working our kidneys are, we can ask the next important question: does alcohol affect kidneys? Simply put: yes! This might not be all that surprising, given that alcohol is a toxin. After all, it’s their job to filter out toxic substances. But let’s take a closer look at 4 specific ways alcohol affects our kidneys:
One significant way alcohol affects our kidneys is by making it more difficult for them to function effectively. For instance, alcohol impairs the structure and function of the nephrons — those functional units of our kidneys responsible for filtering waste products and excess fluids. This can lead to a condition called acute kidney injury, which occurs when the toxins from alcohol build up in our body quickly and our kidneys can’t maintain the right fluid balance. Binge drinking in particular places a great strain on the kidneys and can cause acute kidney damage.
Furthermore, alcohol can affect kidney function by causing or exacerbating other health conditions that harm the kidneys. For example, alcohol is a known risk factor for high blood pressure, a leading cause of kidney damage. Additionally, excessive alcohol consumption can contribute to liver damage and disease, which can, in turn, impair kidney function. Furthermore, alcohol can interfere with the body's ability to regulate fluids and electrolytes, leading to dehydration and electrolyte imbalances that can strain the kidneys.
Finally let’s dispel a myth. Because alcohol is a diuretic, some might think it helps “flush out” the kidneys, but that’s not the case. In fact, it makes them work overtime while depleting the body of important nutrients and damaging the kidneys in the process.
So is beer — an especially potent diuretic — good for your kidneys? The answer is no. Just like other types of alcohol, beer can put unnecessary strain on the kidneys.
It could mean a kidney infection. Alcohol can also increase the risk of kidney infections, which typically start in the bladder and travel up the ureters to the kidneys. Alcohol impairs the immune system, making it more difficult for our body to fight off infections. Additionally, because alcohol can cause dehydration, this can lead to a higher concentration of bacteria in the urinary tract, increasing the risk of a urinary tract infection (UTI). UTIs that spread to the bladder may cause kidney pain and lead to a kidney infection.
Excessive alcohol consumption has been linked to an increased risk of developing chronic kidney disease (CKD), a long-term condition characterized by a gradual loss of kidney function. The likelihood is greater for individuals who already have other risk factors for the disease, such as high blood pressure or diabetes. Smokers who are heavy drinkers have about five times more chance of developing CKD than people who don’t smoke or drink alcohol to excess.
What are the first signs? While the symptoms below can be signs of many different conditions, they are some of the typical ones for CKD:
Alcohol can also interfere with the effectiveness of medications used to manage kidney disease and its complications. For example, alcohol can reduce the effectiveness of blood pressure medications, making it more difficult to control high blood pressure, a leading cause of CKD.
While alcohol consumption isn’t directly linked to kidney stones (hardened deposits formed from minerals and salts in the kidneys), research suggests it can contribute to their development and progression. They can be incredibly painful and sometimes require surgical intervention.
Since alcohol is dehydrating, it increases the concentration of minerals in our urine, which elevates the risk of stone formation. This risk is especially high during instances of binge drinking, which quickly depletes the body's water content. This is also why we might experience kidney pain after a night of heavy drinking.
Alcohol can also affect the balance of acid and alkaline substances in the urine. High levels of uric acid can lead to the formation of uric acid stones. Regular and heavy consumption of alcohol, especially beer and spirits, is associated with higher uric acid levels in the body.
Furthermore, alcohol can exacerbate the symptoms of kidney stones. It can increase the heart rate, leading to faster blood flow and potentially pushing the stones into the ureters, causing severe pain and possible obstruction.
It’s important to be aware of all the ways alcohol can affect our kidneys, as we might develop certain symptoms over time that indicate kidney damage — particularly if we’re consuming alcohol heavily over a long period of time. Plus, issues affecting the kidneys can quickly affect the rest of our body, potentially causing problems in multiple organs.
Watch for these signs that indicate we might have alcohol-related kidney damage:
Kidney pain may be felt in the upper or lower back or between the buttocks and lower ribs. The pain may be felt immediately after consuming alcohol or after we’ve stopped drinking. If we’re experiencing any of the above symptoms or suspect we might have kidney damage from alcohol use, it’s important to contact a medical health professional.
So, how is kidney damage treated — is there a cure? Well, that depends. Acute kidney damage caused by binge drinking will typically resolve itself within a few days. The damage can usually be reversed by stopping drinking and allowing our kidneys to recover. Keep in mind, however, that repeated episodes of binge drinking may cause irreversible damage.
As for chronic kidney disease, sadly there’s no cure. Treatment usually involves helping relieve symptoms and preventing it from getting worse. Our doctor might instruct us to manage our blood pressure levels, follow a kidney-friendly diet, and get adequate exercise.
Depending on the severity of our condition, doctors also might prescribe medications to manage symptoms. In extreme cases, CKD can lead to kidney failure, which may require a kidney transplant or dialysis — a mode of therapy in which a machine is used to perform the job of the kidneys. Untreated, complete kidney failure from alcohol will result in death.
The good news is that we have more control over the health of our kidneys than we might think. It’s worth making certain lifestyle changes, given how vital these organs are to our survival. In addition to limiting our alcohol consumption or eliminating it entirely, there are 5 ways we can keep our kidneys healthy and functioning optimally:
Our kidneys play a vital role in keeping us healthy and alive. They filter out toxins and waste and remove excess fluid from our body. Chronic, long-term alcohol consumption can damage our kidneys, leading to chronic kidney disease or failure. Even a single episode of binge drinking can put stress on our kidneys and cause acute kidney damage. Some of the best things we can do to keep our kidneys healthy include limiting our alcohol consumption, drinking plenty of water, eating a healthy diet, staying physically active, limiting our intake of over-the-counter pain relievers, and not smoking.
If you want to give your kidneys a boost by cutting back on your alcohol consumption, consider trying Reframe. We’re a neuroscience-backed app that has helped millions of people reduce their alcohol consumption and form healthier lifestyle habits.

Does that Pinot jive with your Prednisone? We dive into the science behind this potentially harmful combo and offer practical steps to ensure your health isn't on the line. Ready to make informed choices? We thought so!
You’ve had a rough day at work and, after dinner, you find yourself reaching for a glass of wine, hoping to unwind. But then you remember that you’re currently on Prednisone.
We've probably found ourselves in situations like these, faced with a decision: have a drink, take the medication — or both?
This article explores whether it's safe to mix Prednisone and alcohol and the science behind it.
Prednisone is a corticosteroid medication used to suppress our body's immune system, used for conditions such as arthritis, asthma, and severe allergic reactions.
Let's imagine our immune system as a collection of soldiers. Prednisone acts like a high-ranking officer, ordering these soldiers to stand down, easing our body's inflammatory response.
It's crucial to note that while Prednisone is very effective, it can come with a host of side effects, from mild ones (like insomnia and mood changes) to severe ones (like high blood pressure and weakened immunity).
Now, let's add alcohol to the equation. Drinking alcohol is like adding an unruly group of rebels to our imaginary battlefield. They don't listen to the officer's commands and often cause chaos.
In our bodies, alcohol can exacerbate Prednisone's side effects, causing more harm than good. Alcohol increases gastric acidity, leading to stomach issues like ulcers and stomach bleeding, which Prednisone can also cause.
Simultaneously, both substances can harm the liver, the body's primary detoxification organ.
What’s more, drinking while on a long-term Prednisone regimen could lead to osteoporosis, a disease that leads to the weakening and thinning of our bones. This is because Prednisone lowers our bone mineral density, increasing our risk of fractures.
Alcohol impacts the body’s response to insulin and can lead to insulin resistance. This is also the case for Prednisone and other corticosteroids — which means this combo could lead to an increased risk of developing type 2 diabetes.

Another danger of mixing these two is that it might exacerbate whatever underlying condition is driving us to take Prednisone in the first place.
If we drink that glass of wine after taking our Prednisone, and make this a habit, we might experience a range of immediate and long-term symptoms:
While serious reactions are rare, these increase over time if we drink while on long-term doses of Prednisone.
Notably, our bodies may respond differently to the combination, and the severity of symptoms can vary widely. Therefore, recognizing these symptoms early and seeking medical help is crucial.
We've recognized the potential harm in mixing Prednisone and alcohol. What's next? Here are ways we can safeguard our health:
In conclusion, while that glass of wine after a long day is tempting, the potential risks of combining alcohol and Prednisone far outweigh the momentary relief.

Although it isn’t a treatment for alcohol use disorder (AUD), the Reframe app can help you cut back on drinking gradually, with the science-backed knowledge to empower you 100% of the way. Our proven program has helped millions of people around the world drink less and live more. And we want to help you get there, too!
The Reframe app equips you with the knowledge and skills you need to not only survive drinking less, but to thrive while you navigate the journey. Our daily research-backed readings teach you the neuroscience of alcohol, and our in-app Toolkit provides the resources and activities you need to navigate each challenge.
You’ll meet millions of fellow Reframers in our 24/7 Forum chat and daily Zoom check-in meetings. Receive encouragement from people worldwide who know exactly what you’re going through! You’ll also have the opportunity to connect with our licensed Reframe coaches for more personalized guidance.
Plus, we’re always introducing new features to optimize your in-app experience. We recently launched our in-app chatbot, Melody, powered by the world’s most powerful AI technology. Melody is here to help as you adjust to a life with less (or no) alcohol.
And that’s not all! Every month, we launch fun challenges, like Dry/Damp January, Mental Health May, and Outdoorsy June. You won’t want to miss out on the chance to participate alongside fellow Reframers (or solo if that’s more your thing!).
The Reframe app is free for 7 days, so you don’t have anything to lose by trying it. Are you ready to feel empowered and discover life beyond alcohol? Then download our app today!
You’ve had a rough day at work and, after dinner, you find yourself reaching for a glass of wine, hoping to unwind. But then you remember that you’re currently on Prednisone.
We've probably found ourselves in situations like these, faced with a decision: have a drink, take the medication — or both?
This article explores whether it's safe to mix Prednisone and alcohol and the science behind it.
Prednisone is a corticosteroid medication used to suppress our body's immune system, used for conditions such as arthritis, asthma, and severe allergic reactions.
Let's imagine our immune system as a collection of soldiers. Prednisone acts like a high-ranking officer, ordering these soldiers to stand down, easing our body's inflammatory response.
It's crucial to note that while Prednisone is very effective, it can come with a host of side effects, from mild ones (like insomnia and mood changes) to severe ones (like high blood pressure and weakened immunity).
Now, let's add alcohol to the equation. Drinking alcohol is like adding an unruly group of rebels to our imaginary battlefield. They don't listen to the officer's commands and often cause chaos.
In our bodies, alcohol can exacerbate Prednisone's side effects, causing more harm than good. Alcohol increases gastric acidity, leading to stomach issues like ulcers and stomach bleeding, which Prednisone can also cause.
Simultaneously, both substances can harm the liver, the body's primary detoxification organ.
What’s more, drinking while on a long-term Prednisone regimen could lead to osteoporosis, a disease that leads to the weakening and thinning of our bones. This is because Prednisone lowers our bone mineral density, increasing our risk of fractures.
Alcohol impacts the body’s response to insulin and can lead to insulin resistance. This is also the case for Prednisone and other corticosteroids — which means this combo could lead to an increased risk of developing type 2 diabetes.

Another danger of mixing these two is that it might exacerbate whatever underlying condition is driving us to take Prednisone in the first place.
If we drink that glass of wine after taking our Prednisone, and make this a habit, we might experience a range of immediate and long-term symptoms:
While serious reactions are rare, these increase over time if we drink while on long-term doses of Prednisone.
Notably, our bodies may respond differently to the combination, and the severity of symptoms can vary widely. Therefore, recognizing these symptoms early and seeking medical help is crucial.
We've recognized the potential harm in mixing Prednisone and alcohol. What's next? Here are ways we can safeguard our health:
In conclusion, while that glass of wine after a long day is tempting, the potential risks of combining alcohol and Prednisone far outweigh the momentary relief.

Although it isn’t a treatment for alcohol use disorder (AUD), the Reframe app can help you cut back on drinking gradually, with the science-backed knowledge to empower you 100% of the way. Our proven program has helped millions of people around the world drink less and live more. And we want to help you get there, too!
The Reframe app equips you with the knowledge and skills you need to not only survive drinking less, but to thrive while you navigate the journey. Our daily research-backed readings teach you the neuroscience of alcohol, and our in-app Toolkit provides the resources and activities you need to navigate each challenge.
You’ll meet millions of fellow Reframers in our 24/7 Forum chat and daily Zoom check-in meetings. Receive encouragement from people worldwide who know exactly what you’re going through! You’ll also have the opportunity to connect with our licensed Reframe coaches for more personalized guidance.
Plus, we’re always introducing new features to optimize your in-app experience. We recently launched our in-app chatbot, Melody, powered by the world’s most powerful AI technology. Melody is here to help as you adjust to a life with less (or no) alcohol.
And that’s not all! Every month, we launch fun challenges, like Dry/Damp January, Mental Health May, and Outdoorsy June. You won’t want to miss out on the chance to participate alongside fellow Reframers (or solo if that’s more your thing!).
The Reframe app is free for 7 days, so you don’t have anything to lose by trying it. Are you ready to feel empowered and discover life beyond alcohol? Then download our app today!